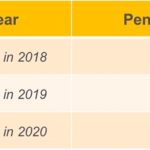
The penalty also remains in effect for 2018 coverage. The only change is the tax penalty will no longer be in effect beginning in 2019.
Covered California Extends Open Enroll Until December 22 For 2018
he plan selection deadline for a January 1, 2018 coverage start date has been extended to Friday, December 22 to accommodate increased interest in enrollment for the new year.
Covered California Keeps Premiums Stable by Adding Cost-Sharing Reduction Surcharge Only to Silver Plans to Limit Consumer Impact
In the absence of a federal commitment to continue funding cost-sharing reduction (CSR) reimbursements through the upcoming year, Covered California health insurance companies will add a surcharge to Silver-tier products in 2018. However, because the surcharge will only be applied to Silver-tier plans, nearly four out of five consumers will see their premiums stay the same or decrease, since the amount of financial help they receive will also rise. Those who do not get financial help will not have to pay a surcharge.
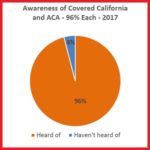
New Survey Highlights Continued Need for Marketing of Health Insurance
In addition, the study found that the political debates in Washington had spurred uncertainty among the uninsured and those who have a health plan through Covered California. However, while nearly two-thirds of those surveyed reported they were concerned about the future of Covered California and the Affordable Care Act, four out of five still plan to renew their coverage.
New Analysis Shows the Graham-Cassidy Plan Would Force Millions to Lose Coverage and Threaten to Collapse California’s Individual Market
“The Graham-Cassidy plan takes resources away from California and from the majority of states, which means that far fewer Americans would have insurance or the existing protections from insurers,” said Peter V. Lee, executive director of Covered California. “The effect on California would be devastating, and lead not only to there being more uninsured people than there were before the Affordable Care Act, but would also cause huge negative impacts on the health care delivery system, the economy and on those with employer-based coverage.”
Children To Get Hit With Higher Health Insurance Rates In 2018
Since 2014 under Affordable Care Act rules, new ACA qualified health plans had just one rate for dependents from ages 0 to 20. In 2018 there will now be 7 different age based rates with the first for ages 0 – 14. Beginning at age 15 there will be a separate age rates per year up to age 20. The new member level age rating does not apply to grandfathered plans.
Covered California: Marketing and Outreach to Stabilize the Individual Market Report
“A comprehensive marketing and outreach campaign has been a critical ingredient of Covered California’s success, and more importantly is a vital component of any effort to promote stability in individual markets across the nation,” said Lee. “Getting the word out is a proven way to promote enrollment and bring more healthy people into the risk pool, which lowers premiums and saves money for everyone.”
WHA Expands To Bay Area, But Leaves Covered California
Western Health Advantage (WHA) has announced that the Department of Managed Health Care has approved their expansion for small group plans into the Bay Area. They also noted that they will not seek re-certification of their Covered California small group plans because of this expansion. WHA’s exit from the Covered California for Small Business plans does not affect their individual and family plan offerings through Covered California.
Covered California Releases 2018 Rates, Plans, And Carriers
Covered California instructed health insurance companies to submit their rates assuming direct payment to fund the CSR subsidies would be continued, but to also submit a separate CSR surcharge to “load” any costs to fund this program onto Silver-tier plans for those who receive subsidies. As a result, Silver-tier consumers may see an additional “CSR surcharge” that averages 12.4 percent — ranging from 8 percent to 27 percent on the gross price of their premiums
Covered California Board Approves Silver Plan Rate Spike For 2018
Covered California’s board acted to place any rate increases caused by the uncertainty only onto Silver plans. While Silver level consumers will see an increase in the gross cost of their premiums, they will also see an increase in the amount of financial assistance they receive, leaving their net payment virtually the same.
- 1
- 2
- 3
- …
- 11
- Next Page »