
Covered California may not have generated a 1095-A if your account had been withdrawn during 2014.
2016 1095-A Tax Premium Tax Credit Statements
Covered California states that they started processing the 2016 1095-As as of January 5, 2017. The form should be in the consumer’s Covered California account Summary>Documents and Correspondence>CalNOD62A_IRSForm1095A_2016 by the end of January. The form should also be mailed out to consumers at the address listed for receiving mail.
New – Covered California Issues Revised 2016 1095-As
Covered California Guidance For Obtaining 2016 1095-As
[wpfilebase tag=list id=389 pagenav=1 /]
1095-As for 2015
1095-As from Covered California and 1095-Bs for Medi-Cal enrollments should be sent by January 31, 2016. If you have not received a 1095-A from Covered California in the mail or through your Covered California account you can either call 1-800-300-1506 or file an online dispute form at
Covered California 1095-A Dispute Form
Medi-Cal 1095-Bs will be sent by the Department of Health Care Services. For more information on the Medi-Cal 1095-Bs visit
http://www.dhcs.ca.gov/services/medi-cal/eligibility/Pages/1095_QA.aspx
Employer sponsored small group health insurance 1095-Bs may not be sent out until the end of March.
Other documents that may assist you in determining which 1095 forms you need-
[wpfilebase tag=browser id=224 /]
2014
A handful of people have reported that they have not received their Covered California 1095-A Health Insurance Marketplace Statement. As I researched what may have happened to these missing forms I noticed all the people who had not receive their 1095-A also had their Covered California application withdrawn at some point during 2014. The only way to get a 1095-A if it has not been generated and sent from Covered California is to fill out their 1095-A Dispute and send it to Covered California.
March 20, 2015 Update: IRS waives ACA premium taxes
The Treasury Department has decided to expand their February 24 announcement waiving collection of under reported health insurance tax credits to states that are running their own Marketplace exchanges. Tax payers who already filed their tax returns using incorrect 1095-As issued by Covered California will not be subject to the collection of excess Advance Premium Tax Credits (APTC) not reported on the 1095-As. This is a very limited decision by the Treasury Department and does not vacate the responsibility of tax payers waiting for a corrected 1095-A to from repaying any APTC they may owe. Read more with down loads -> IRS waives tax collection from incorrect Covered California 1095-As
March 16, 2015 Covered California Update
Covered California issued a news brief related to their progress to issue correct 1095-As and send out the important IRS form for people who have not received them. In short-
- Starting March 16th, 2015, Covered California will begin calling people who have filed the 1095-A dispute form and notifying them of the status. (I assume if you get a phone call instead of a correct 1095-A that means they have either denied the dispute or they need more information.)
- Consumers should check their secure Covered California inbox to see if a corrected 1095-A has been sent. The letter will indicate it is a NOD-62B for corrected 1095-A.
- If a consumer hasn’t heard from Covered California after 60 days, they should call and find out what the heck is taking so long.
- Consumers who NEVER received a 1095-A should check to make sure they Covered California has their current and correct address. They should also immediately file the 1095-A Dispute Form. ([wpfilebase tag=fileurl id=433 linktext=’1095-A Dispute Form Covered California’ /])
For a copy of the full news brief download –
- [wpfilebase tag=fileurl id=621 linktext=’March 16th_Importantant Update to missing and corrected 1095-As’ /]
10,000 Californians without 1095-As
California Healthcare Foundation Center for Health Reporting quoted Covered California’s Dana Howard as stating that there are an estimated 10,000 tax filers who have not received a 1095-A at all. Covered California is blaming the lack of the crucial tax document on conflicting account information. See the full story at Obamacare’s tax-time lessons by Emily Bazar
Is my 1095-A lost in the mail?
I recently received a comment on my blog post Getting a corrected 1095-A from Monica who wrote,
I have been told by Covered CA that I will not receive a form 1095A because my application was withdrawn in April of 2014. At that point I created another CC account and enrolled in a Silver plan. They are telling me that because the app was withdrawn (by one of their reps) that no form 1095A will be generated.
They have advised me to file a dispute form that can take up to 60 days to resolve, leaving me near the filing deadline. And that even then I may not get a 1095A.
Was your application withdrawn in 2014?
Covered California customer service representatives would routinely withdraw an enrollment when it seemed hopelessly screwed up and the best course of action was to start all over again. Withdrawing an application is different than terminating participation. You terminate a plan to end in the future such as when the individual might be gaining group coverage or ageing into Medicare. The act of withdrawing an application can erase the enrollment retroactively to the beginning effective date.
2014 enrollment information wiped out
The act of withdrawing a application, at least for the client’s I reviewed, has wiped out their 2014 enrollment data. When I toggle to view 2014 data in the Covered California CalHEERS program, it doesn’t show that the individual or family was ever enrolled. With no enrollment, there is no data to report on a 1095-A such as the SLCSP or Tax Credit. Covered California has told me the data is floating around somewhere in their system. That’s so reassuring.
IRS showdown
I have seen Covered California withdraw applications to reset an account after it was improperly deemed Medi-Cal and they just needed to start the enrollment anew. Covered California also withdrew an application of family whose health plan seemed tied in knots because the carrier could get the details straight. In both of these instances a 1095-A has NOT been generated. In all these cases, the consumer paid premiums to health plans and Covered California paid tax credits to the health plans to lower the premiums. Covered California has to generate 1095-A’s for these taxpayers because they made them promise to file federal taxes and they can’t do that without the 1095-A.
Filing an amended return
From the blog Getting a corrected 1095-A, Monica also reported,
CC advised me to file with what I have while they are researching my dispute form. She said I will then have to file an amended return.
If Covered California is going to force these taxpayers to file an amended return because the CalHEERS program screwed up and wiped out their enrollment delaying the generation of a 1095-A, Covered California ought to pay for the extra tax preparation fees of filing an amended return.
Is the 1095-A online?
It is easy to determine if a 1095-A has been generated but not received in the mail by checking the Documents and Correspondence section of the Summary page on your Covered California account. The document CalNOD62AIRSForm1095A should have been generated no later than January 24th. If this file is in your account you can download it to your computer to use with filling out your federal taxes. If no 1095-A document exists, you’ll have to file a 1095-A Dispute Form with Covered California to get one generated. Download the 1095-A Dispute Form at the end of the post.
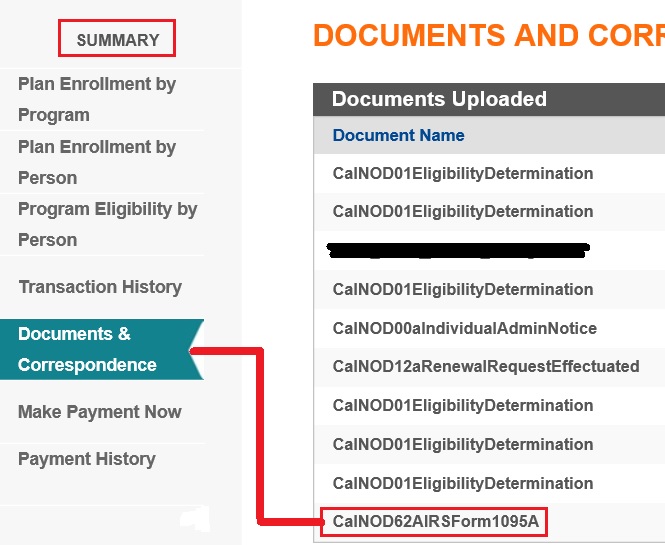
The 1095-A can be found in the Documents & Correspondence section of the Summary page of the Covered California account.
- [wpfilebase tag=fileurl id=433 linktext=’1095-A Dispute Form C…’ /]


