Covered California has found an error in the calculation of the 2026 subsidy for health insurance premiums. While they have fixed the error, it appears that the health plans must claw back the subsidy overpayments beginning in March.
Covered California consumers may only have been made aware of the excess subsidy error when they received abnormally high health insurance premium invoices for March. If you opted not to receive paper notifications, the email is in your Covered California secure email box. The notification states,
While preparing for the 2026 benefit year, we identified an issue affecting the calculation of your federal premium tax credit.
We have fixed the issue and notified your health insurance company.
The following sentence indicates that overpayment of subsidy began in January.
The correct amount is included in this notice and will be applied to your enrollment on 1/1/2026.
Lower Subsidy and Claw Back by Health Plans
In other words, incorrectly high subsidy paid to the health plans must be repaid back to the health plan. This is leading to March invoices larger than just the recalculated subsidy because the consumer must pay the higher premium plus repay the excess subsidy for the prior months.
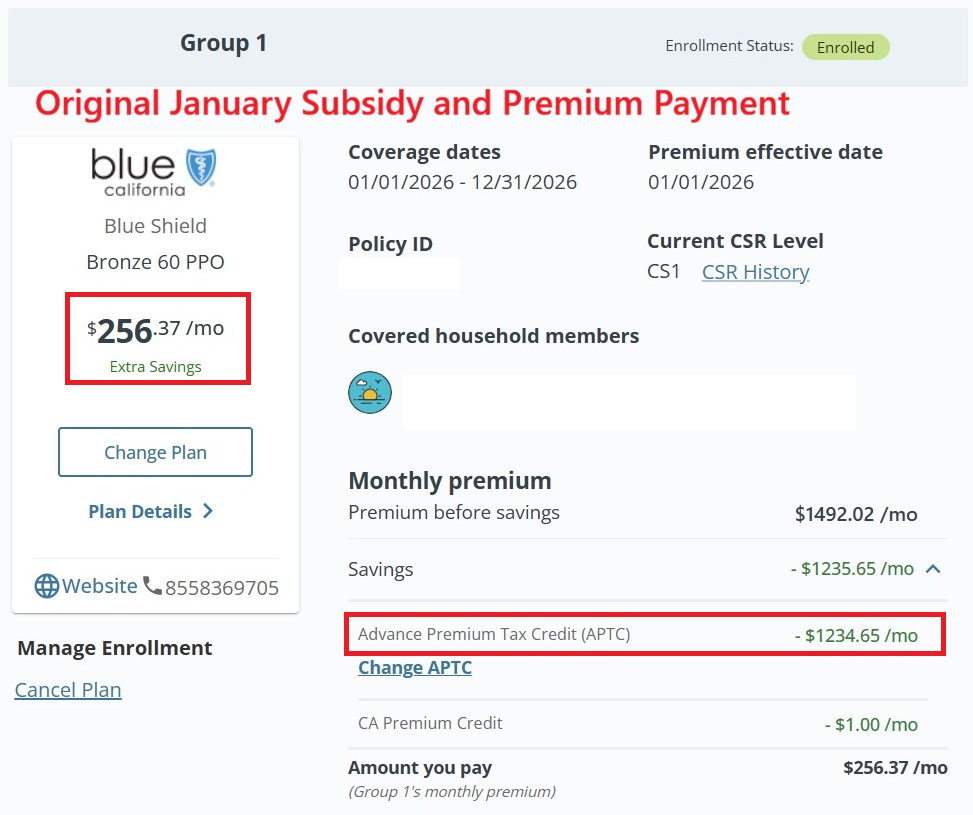
In December 2025, this consumer enrolled in Covered California and received a subsidy (APTC) of $1,234.65 a month making their health insurance premium $256.37.
After Covered California discovered the subsidy calculation error, they had to lower the monthly subsidy amount by $19.21. This made the new health insurance premium $275.58. However, the March invoice was higher than the premium shown on the Covered California Enrollment Dashboard.
It appears the health plan invoiced for the higher premium plus the excess subsidies paid in January and February. Consequently, the March invoice was $314.00 the combination of $275.58 + $19.21 + $19.21.
The April invoice should drop down to the recalculated premium of $275.58. The health plan must claw back the excess subsidy because Covered California is clawing it back from the health plan.
I reached out to both Covered California and the health plan regarding the subsidy and higher invoices and no one gave me any answers. We don’t know if the subsidy error was because of the One Big Beautiful Bill, new regulations at the federal level, or a software issue within the Covered California CalHEERS program.
Additionally, Covered California has not said if the subsidy error is disproportionately occurring for higher or lower income consumers. All we know is that some Covered California consumers will have larger health insurance invoices as the subsidy is recalculated lower and they must repay the health plans the excess subsidy applied to their enrollments that began in January 2026.
YouTube video reviewing the subsidy error.