2025 IFP
Blue Shield adds Virtual PCPs and Amazon Pharmacy
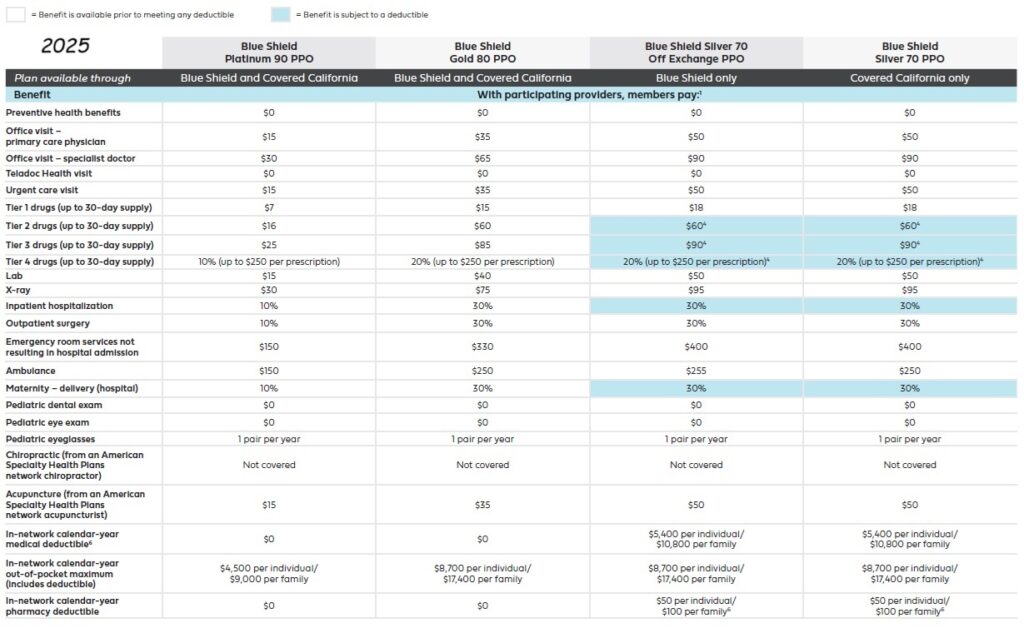
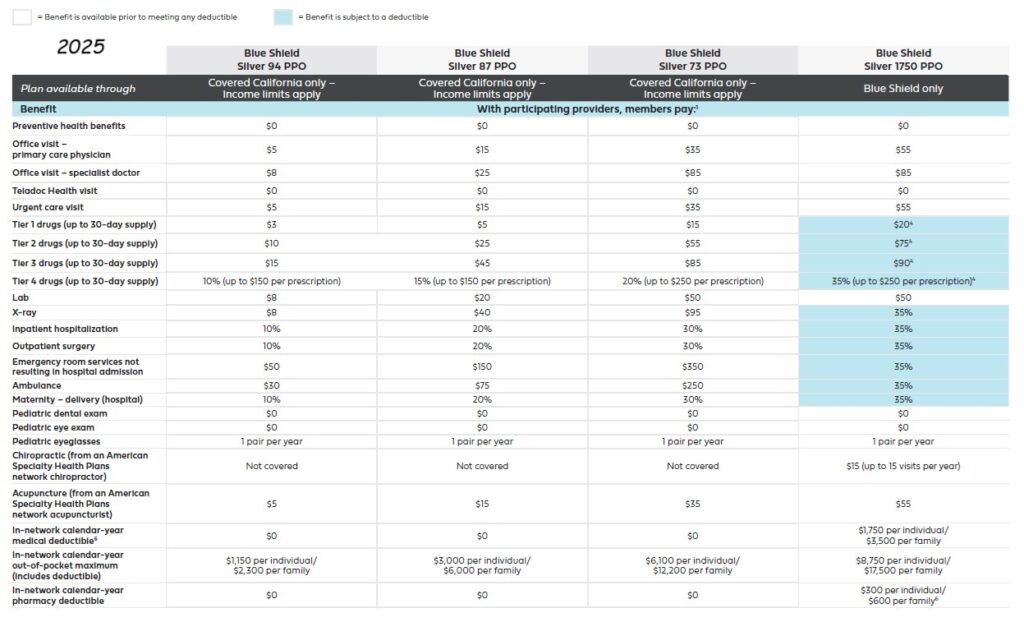
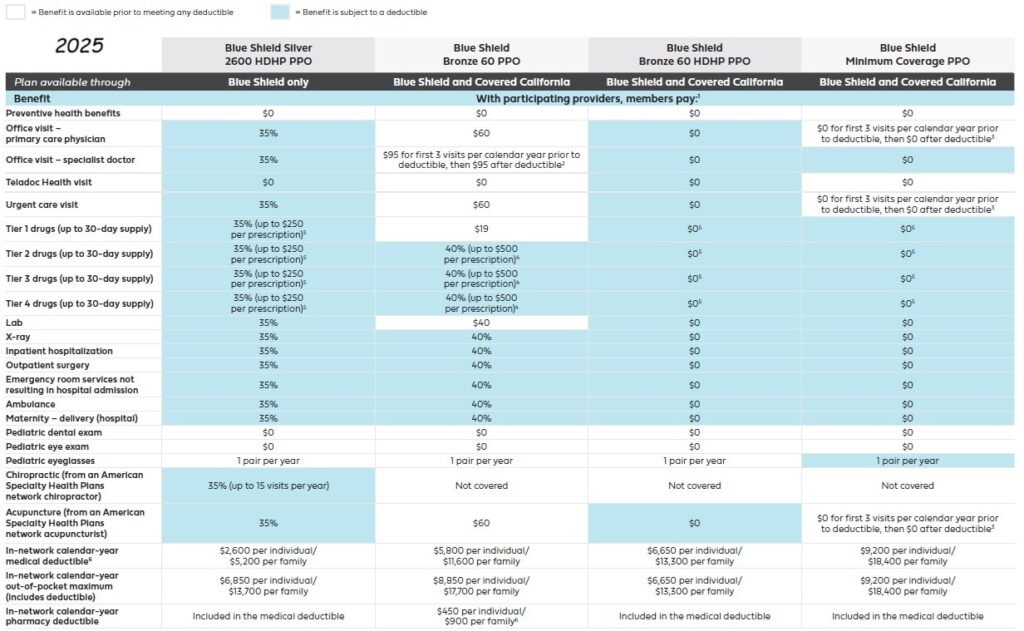
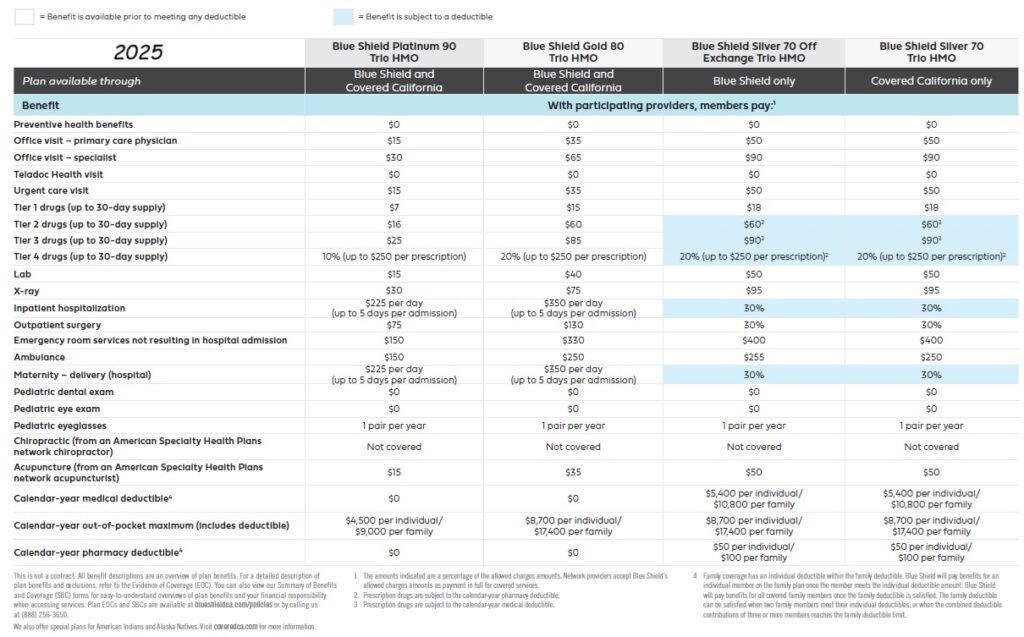
2025 Plan Documents Blue Shield IFP
2024 Blue Shield Individual and Family Health, Dental and Vision
Stanford Health Care Out-of-Network with Blue Shield plans, click to read more.
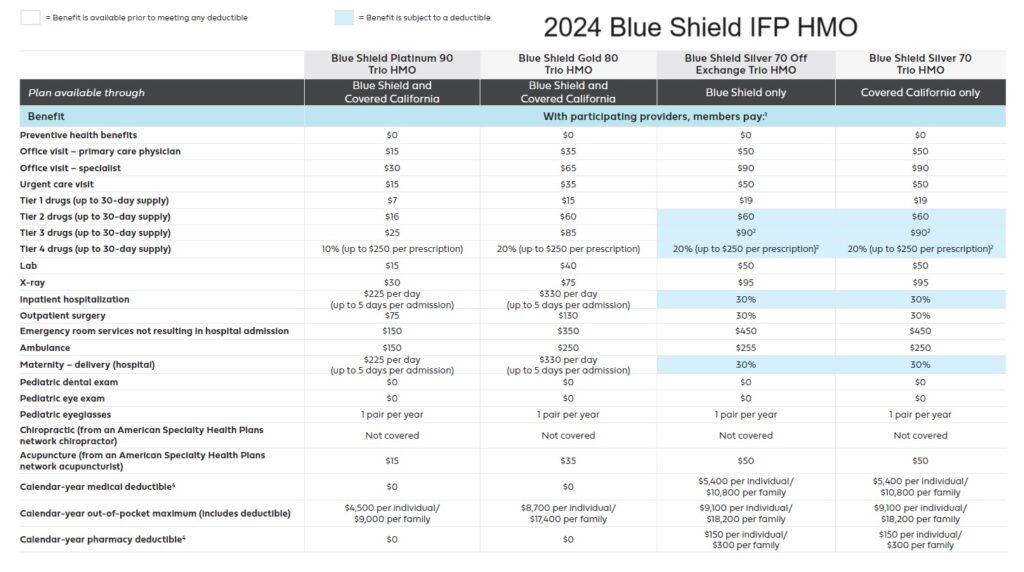
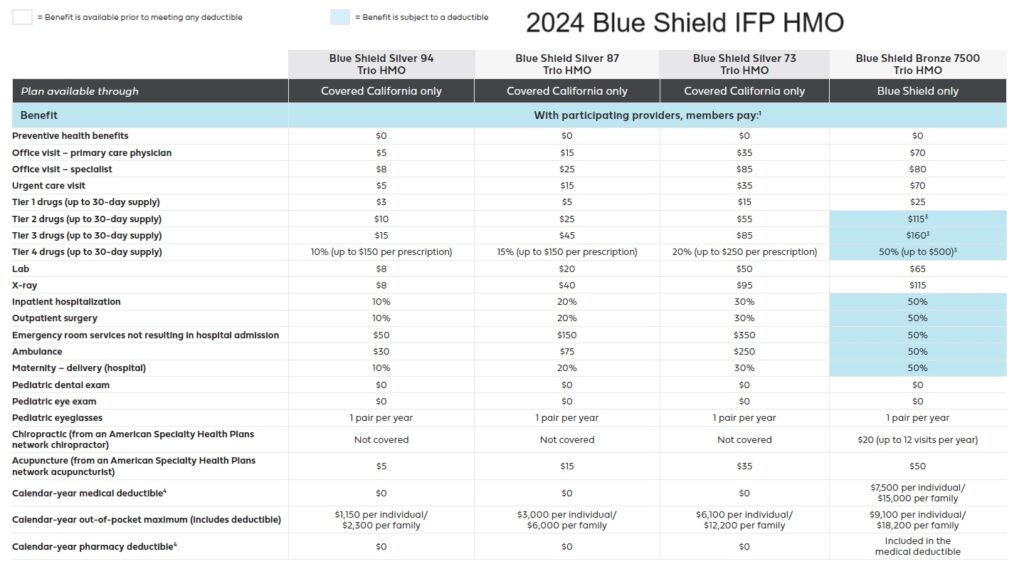
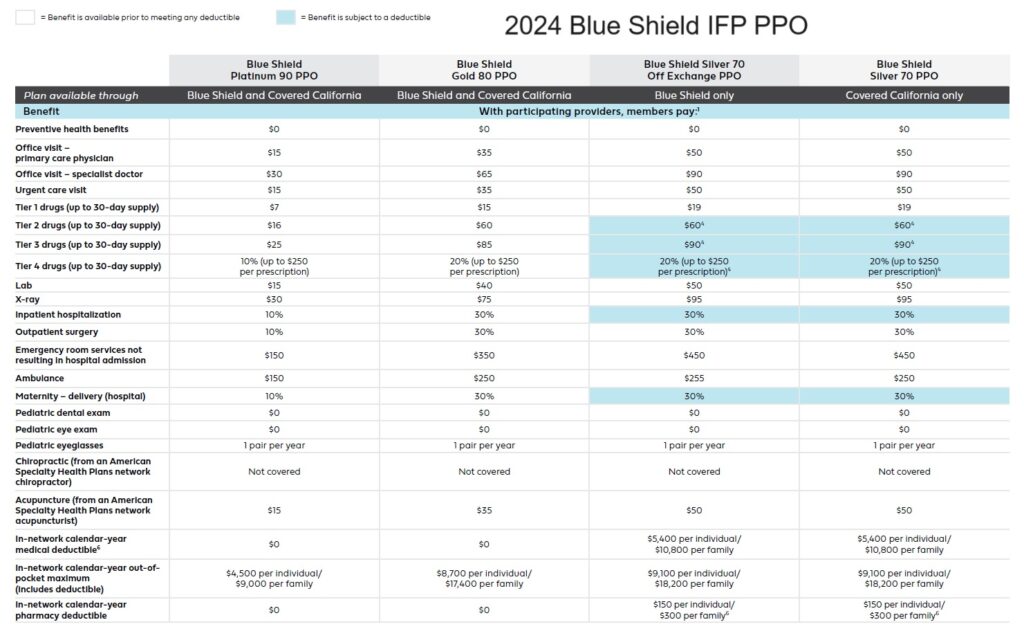
2024 Blue Shield IFP
2023 Blue Shield IFP
Medical ID cards go digital in 2021
In October, we expanded our Go Paperless initiative by offering digital medical ID cards for members who opt in for paperless electronic communication. Digital medical ID cards contain the most up-to-date information and are easily accessible at blueshieldca.com. Members can also use their mobile device to download the Blue Shield of California mobile app on the App StoreSM or Google PlayTM.
- The impacted members include:
- All off-exchange applicants who applied in 2020 and 2021
- All members on autopay
- All members who have registered for Teladoc
- Members who opted into electronic delivery between 2018 and October 2020 received digital medical ID card effective January 1, 2021. Members can access their medical ID cards for individuals and the family through the online portal whether they opted for paperless or not.
- Members who selected paper delivery as their preference for medical ID card continue to receive printed medical ID cards.
- Dental and vision products: new and existing members continue to receive printed ID cards for dental plans through the dental carrier. For vision plans, members do not need ID cards and can have providers confirm through mesvision.com/providers or call (800) 877-6372.
- Members who would like a printed medical ID card may request through the Blue Shield member portal at their convenience.
October 30, 2020
Blue Shield of California continues to grow its Trio HMO network in Southern California. We are happy to share a new addition in the Inland Empire and remind you about other Trio HMO additions we previously announced in Los Angeles, Riverside, San Bernardino, and Ventura Counties effective January 1, 2021. This applies to all lines of business that offer Trio HMO.
Allied Pacific IPA has added Alpha Care Medical Group to our Trio HMO network. Allied Pacific IPA, founded in 1992, is committed to providing quality and patient-centered medical care through an extensive and accessible network of healthcare professionals. Alpha Care adds another 102 physicians in the Inland Empire.
PrimeCare will now include San Bernardino Medical Group, PrimeCare of San Bernardino, PrimeCare of Redlands, and PrimeCare of Hemet Valley to our Trio HMO network. The addition of these medical groups adds over 50 additional physicians in the Inland Empire.
PIH Health is a nonprofit, regional healthcare network that serves approximately 2.5 million residents in Los Angeles County. The fully integrated network is comprised of PIH Health’s medical group and three hospitals in the cities of Los Angeles, Whittier and Downey. PIH Health adds network depth to the south and east Los Angeles area with 390 full time physician providers, plus 300 more physicians in their affiliated network.
Valley Care IPA joins the Trio HMO network in Ventura County with 106 affiliated primary and specialty care physicians. Established in 1994, Valley Care IPA’s goal is to provide local families with a choice of physicians practicing throughout Santa Paula, Fillmore, Camarillo, Oxnard, Ventura, and neighboring communities.
Blue Shield Provider Search Tool
- Make sure to select the correct year and plan type before searching for a provider such as a doctor or hospital.
Exclusive PPO Network statewide
All Blue Shield of California individual and family plans will be Preferred Provider Organization (PPO) types that allow members to receive services from providers outside of the new Exclusive PPO Network. All plans offered through Covered California will adhere to the 2016 Standard Benefit Design. The same plans will be offered off-exchange directly from Blue Shield for individuals and families who do not qualify for the tax credits. In addition, Blue Shield of California will offer three non-standard benefit design plan in Silver and Bronze metal levels off-exchange.