 Children’s dental insurance options have now been added to the line of plans being offered through California’s health insurance exchange Covered California. Part of the ten Essential Health Benefits that must be offered through the new health insurance exchanges or Marketplaces is pediatric dental. The state exchanges can meet this requirement in various ways and Covered California has opted to offer stand alone plans.
Children’s dental insurance options have now been added to the line of plans being offered through California’s health insurance exchange Covered California. Part of the ten Essential Health Benefits that must be offered through the new health insurance exchanges or Marketplaces is pediatric dental. The state exchanges can meet this requirement in various ways and Covered California has opted to offer stand alone plans.
Children’s dental insurance gets added to health plan offerings
Six different insurance companies will be offering pediatric dental health plans through the Covered California marketplace:
| DHMO | DPPO | DEPO | |
| Anthem Blue Cross | X | ||
| Blue Shield | X | X | |
| Delta Dental | X | X | |
| Health Net | Opted | Out | |
| LIBERTY | X | X | |
| Premier Access | X | X | |
| DHMO: Dental Health Maintenance Organization | |||
| DPPO: Dental Preferred Provider Organization | |||
| DEPO: Dental Exclusive Provider Organization | |||
Most dental plans offered through out California
Not all plans and types will be available in all 19 regions of California and there may be further restrictions based on counties within the region. Each region will have at least five different plans to choose from. The monthly premiums will also vary by region. While most of the plans can be selected separately, Health Net plans are bundled with their health insurance. This means you could select Blue Shield for health insurance and Premier Access for your children’s dental plan. Conveniently, it will all be billed together.
All plans cover preventive at no cost
The plans being offered are all priced pretty close to what an individual dental plans costs today. All the plans include recommended cleanings, x-rays, exams and sealants at no charge. The cost for the other services will depend on whether you choose a Dental Preferred Provider Organization (DPPO) plan type or a Dental Health Maintenance Organization (DHMO) plan type.
 Freedom to choose
Freedom to choose
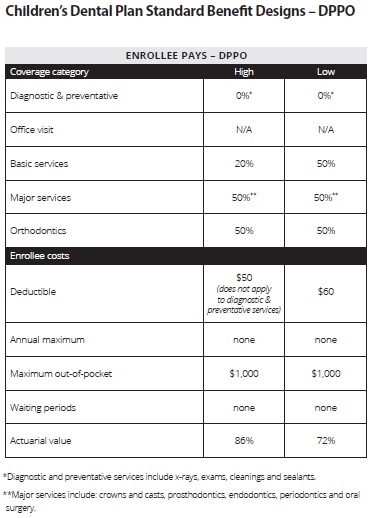
DPPOs allow you to go to any dentist in the network and some cost sharing for dentists out of the network. The cost of services above and beyond the preventives of cleaning, exam and x-rays, are based on a shared percentage. To have a regular cavity filled you might pay 20% and the insurance pay 80% of the cost. DPPOs will have a deductible like $50 that has to be met and they will cap there yearly contribution towards dental services at $1,000
 Predictable costs
Predictable costs
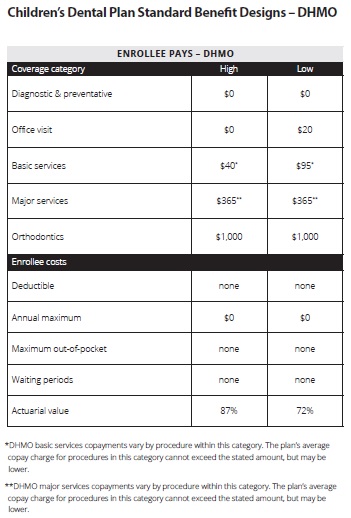
DHMOs usually have lower monthly premiums, but some plans will charge for an office visit. Instead of a set cost sharing percentage for different services, DHMO’s use a flat copayment. These copayments will vary with the type of service like crowns and root canals. Unlike DPPOs, you must select a dentist to enroll with and there is no coverage for services from an out-of-network dentist. DMHOs don’t have a deductible you have to meet and there is no yearly maximum cap on services.
Exclusivity
Dental Exclusive Provider Organizations (DEPOs) are almost exactly like the DPPO. The big difference is no coverage for services provided by dentists outside of the exclusive network. But you are free to see any dentist within the network for routine services, unlike the DHMO plans that lock you into a dentist unless you actively request a change with the insurance plan.
High and Low plans
Each DPPO and DHMO plan will have a “High” and “Low” option. The High plan option will carry a higher monthly premium but the cost sharing or copayments will be less. The High plan is expected to cover 85% of average annual costs and the Low plan is predicted to be 70%. These are actuarial values meaning that of the pool of members in either pool, the average child that actually need dental services will have either 70% or 85% of his or her services covered by the respective plan.
 Monthly premiums
Monthly premiums
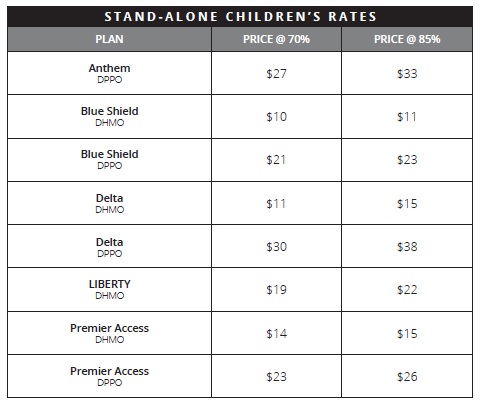
Monthly premiums for Region 3 (Sacramento, Placer, El Dorado, Yolo counties) are fairly typical of the other regions. These plans and premiums will be available to children up to 19 years of age. The premiums for the child dental plans are eligible for the Advance Payment Tax Credit.
Download Covered California Children’s Dental Plans, Rates and Regions [wpdm_file id=78]
September 16, 2013 Update
Covered California has signed contracts with the providers of pediatric dental plans. While they said only “stand alone” plans would be available, Health Net had bundled the children’s dental with their health plans. Covered California has struggled with the “stand alone” versus bundle option and has come down on the side of only making children’s dental plans as “stand alone” option. This has led Health Net to drop the pediatric coverage in their health plans. The press announcement notes that Covered California will continue to work toward a solution of embedding or bundling the pediatric essential health benefit for all health plans in 2015. Read the full announcement below –
COVERED CALIFORNIA FINALIZES CONTRACTS
FOR CHILDREN’S DENTAL PLANS IN 2014
Board Directs Exchange to Expand Options in 2015,
Points to Embedded Model as Best Option
SACRAMENTO, Calif. — Underscoring its commitment to children’s oral health, Covered California™ announced today that insurers signed contracts to offer pediatric dental coverage in 2014 in both the Exchange’s individual and small-group employer markets.
The contracts offer stand-alone plans for children’s dental coverage in the first year of the new health benefit exchange, which will open for enrollment Oct. 1. Meanwhile, Covered California pledged to work toward embedding pediatric dental coverage in its 2015 portfolio of comprehensive medical insurance products.
Five insurance companies will offer plans to families who buy insurance through Covered California in 2014: Anthem Blue Cross, Blue Shield of California, Delta Dental, Liberty Dental and Premier Access.
Seven companies will offer plans in Covered California’s Small Business Health Options Program (SHOP): Blue Shield of California, Delta Dental, Guardian, Liberty Dental, MetLife, Premier Access and Safeguard.
The companies offer a rich mix of plan choices statewide with rates as low as $8 per month in some areas.
In a special meeting Aug. 8, the Covered California Board voted to direct staff to come back by the end of the year with proposals for embedding children’s dental coverage in all Covered California health insurance plans in 2015. Covered California has begun reviewing how that could be accomplished under federal and state laws, while engaging consumer and dental care advocates.
Because of technical constraints, Covered California is unable to offer bundled pediatric dental plans in 2014. This has led to Health Net’s withdrawal from participation in Covered California’s 2014 pediatric dental plans. However, Health Net will participate in the offering of Covered California health plans in the individual and small-group markets for 2014.
Covered California does not expect any pediatric dental coverage gaps, as the remaining plans are well-positioned to offer a variety of stand-alone coverage choices to families in each of the state’s rating regions.
###
Covered California News Release
COVERED CALIFORNIA ROLLS OUT PLANS FOR CHILDREN’S DENTAL COVERAGE
More Children Will Have Access to Improved Care Through a Diverse Choice of Plans, Products and Premiums
SACRAMENTO, Calif. — Covered California™ announced its selection of pediatric dental health plans, ensuring that California children up to 19 years old will get expanded opportunities for better dental health.
With its release of these plans and rates, Covered California took another step toward fulfilling the mandates of the historic federal health care reform law, the Patient Protection and Affordable Care Act, aimed at closing the health insurance gap for millions of Americans.
“These plans dovetail with our mission to make sure every person in the state — and particularly our youngest and most vulnerable — get improved health care,” said Covered California Executive Director Peter V. Lee.
The six selected companies are, Anthem Dental, Blue Shield of California, Delta Dental of California, Health Net Dental, LIBERTY Dental Plan and Premier Access Dental. The products include stand-alone plans, and all can be bundled with health insurance for a single premium.
Nine stand-alone plans are being offered by five issuers, while Health Net Dental is available only in a bundled option.
Three different product types are available, depending on where the child lives: dental health maintenance organizations (DHMOs), dental preferred provider organizations (DPPOs) and dental exclusive provider organizations (DEPOs). Like Covered California’s health insurance plans, the pediatric dental plans underwent a rigorous screening and competitive bidding process and had to balance access to providers with affordable premiums to qualify.
The dental plans feature a diverse mix of large, multistate insurers and smaller, locally based companies. Stand-alone plan premiums range from less than $10 a month for an HMO plan in some areas to about $30 a month for a DPPO.
“Purchase of the pediatric dental benefit is not required. However, the plans offer comprehensive child dental coverage, particularly important for consumers of child-only coverage and family plans,” Lee said. “Dental care is a vital component of overall health, and especially critical for our state’s children. Access to dental services as a youngster means better health, both for children and as they get older.”
Covered California dental benefit plans feature standard copayments, deductibles and coinsurance requirements. Unlike Covered California’s health insurance plans, dental plans are not designated by metal levels, but come in two actuarial value options: 85 percent, which features higher premiums but lower average out-of-pocket costs; and a 70-percent value plan, with lower premiums and higher average out-of-pocket costs.
### End ###

