2018 Individual & Family Plans
While Covered California has released their rate booklet of participating health plans for 2018, as of September, none of the carriers have released specific information about their networks and drug formularies. We know that Anthem Blue Cross will only be offering plans in Regions 1, 7, and 10, meaning most of the Bay Area, Sacramento, and Southern California will not have access to Blue Cross Plans. Health Net is introducing a new narrow network PPO, but we are still waiting for additional provider network details. As this information becomes available I will post it here and on the specific carrier pages on this website.
2017 Covered California Health Plans
The first thing to remember is that all the health plans within a specific metal tier level and benefit design are standard across all the health insurance companies. In other words, the benefits and member cost sharing of a Silver 70 plan are exactly the same regardless the insurance company. The deductible, copayments, and coinsurance are exactly the same. At a high level view, the only difference between the health plans is the monthly premium rate, they type of plan (EPO, HSP, HMO, PPO), and the providers in the plans network.
2017 Standard Health Plan Benefit Design
[wpfilebase tag=file id=1607 /]
What is the difference between and EPO, HSP, HMO, PPO?
Hospitals In-Network by Health Plan by Region/County
Providers
For many consumers, a top priority is keeping the doctors, hospitals and other providers in-network. Each carrier has an online provider search tool to see which doctor are in-network with the plan. Unfortunately, the online tools can be complicated and may not show a doctor as in-network when really he or she is.
Online Provider Search Tools are Horrible
Quality Ratings
Covered California has quality star ratings underneath each of the plans, but I don’t put much faith in these ratings. Most of the data is administrative and not necessarily relate to health care services. Kaiser usually gets very high marks for their health plans. Consumers either love the Kaiser Permanente HMO model of health care or they don’t. Those who don’t like Kaiser are not members. Consequently, the survey to determine the quality of the Kaiser health care services is derived from people who like Kaiser and stay with the plan.
The California Office of Patient Advocate has released 2016 quality ratings on various health plans.
2016 Health Plan Quality Report Card Ratings
2016 – 2017 HMO Quality Ratings
2016 – 2017 PPO Quality Ratings
Medical Groups
Medical Groups are organizations of doctors that are contracted by HMO plans. A member selects a Primary Care Physician who then makes referrals within the medical or physicians groups for specialty health care services. Most HMO plans will have a couple different medical groups within the plan, excluding Kaiser who only supports the Kaiser medical group of doctors. Some of the health plans have not made it easy to determine which medical groups are participating in their HMOs. But if you can find out the medical groups, the Office of Patient Advocate also has some quality ratings a variety of large medical groups through out California.
Evidence of Coverage
The Evidence of Coverage (EOC) or Member Agreements are the guide books on how the plan operates. They are also the contract between the health plan and the member. They spell out how health care services are obtained, limits, exclusions, along with pediatric dental and vision benefits. The EOCs are long documents but have important information. This is where the devil is in the details. I have tried to post the EOCs and Member Agreements as they become available for the new year under each health plans page. Unfortunately, not all the carriers have posted their EOCs. Health Plan Pages
Drug Formularies
Drug formularies are the list of prescription drugs a health plan will cover under the prescription drug benefit. If you are taking a specific brand name medication, it is worth the time to check out the latest drug formulary for the plan to see if it is covered and at what pricing tier. Some brand name drugs maybe listed for one carrier but not the other. Or, it might be listed at a different pricing tier, such as Tier 2 or Tier 3. This all affects the out-of-pocket costs for the member.
Older information on comparing health plans
Several of the health plans selected to be part of the Covered California health insurance market place have never been heard of beyond the ethnic community or region they serve. In addition, many of the plans have no experience with offering commercial individual health insurance plans. Will these regional plans be up to the task of offering and managing health insurance to a possible flood of new members?
Covered California health plan historical data
It’s hard to compare the plans side by side because of the diversity of populations they serve and lack of data on some of the health insurance organizations. Much of the information about the different health plans and companies is spread out over several different agencies, reports and websites. Most of the insurance companies are involved in several different types of insurance products from commercial individual and group to government sponsored Medi-Cal or Medicare.
| Plan | Members | Medicare | Medi-Cal | Healthy Families | Group | IFP |
| Alameda Alliance For Health | 140,000 | X | X | X | ||
| Anthem Blue Cross | 4.5 million | X | X | X | X | X |
| Blue Shield of California | 3 million | X | X | X | ||
| Chinese Community Health Plan | 14,300 | X | X | X | ||
| Contra Costa Health Services | 80,000 | X | X | X | X | |
| Health Net | 1.8 million | X | X | X | X | X |
| Kaiser Permanente | 6 million | X | X | X | ||
| L.A. Care | 1 million | X | X | X | ||
| Molina Healthcare | 198,000 | x | X | X | ||
| Sharp Health Plan | unknown | X | ||||
| Valley Health Plan | unknown | |||||
| Ventura County Health Care Plan | unknown | X | ||||
| Western Health Advantage | 92,000 | X | X |
- Members: California membership in the various plan types estimated from available online reports.
- Group: small and large employer group plans in the commercial market.
- IFP: individual and family plans in the commercial market.
Small foot print of information
Some of the plans have a very little information, other than their website, because the population and region they serve is relatively small. Consequently, there may only be one report or rating available as a guide post on how the health plan will perform. Government sponsored plans such as Ventura County Health Plan and Valley Health Plan have virtually no data on them at all compared to the larger insurers in California. Past performance may not be indicative of how a plan will serve members in the new Covered California health plans.
Available public information
There are two bureaucracies that regulate health insurance in the state:
1. California Department of Managed Care (CDMC) regulates all HMO plans plus some PPO plans of Blue Cross of California and Blue Shield of California. (The Blues are two separate and distinct companies in California)
2. California Department of Insurance regulates PPO plans offered by various companies.
CDMC enforcement actions
Enforcement actions reported by CDMC since July 2000. When reviewing the information remember that some insurers only have 15,000 members while others may have millions of members. Even though these enforcement actions are for HMO plans which might not be offered by the specific insurer through Covered California, these are actions that usually speak to the administration of plans. The link is to the CDMC enforcement action page for the insurer and the number indicates how many enforcement actions have been recorded.
| Alameda Alliance For Health 4 |
| Anthem Blue Cross 770 |
| Blue Shield of California 212 |
| Chinese Community Health Plan 2 |
| Contra Costa Health Services 2 |
| Health Net 150 |
| Kaiser Permanente 193 |
| L.A. Care 7 |
| Molina Healthcare 7 |
| Sharp Health Plan 8 |
| Valley Health Plan none found |
| Ventura County Health Care Plan 3 |
| Western Health Advantage 2 |
California Department of Insurance also has a searchable data of enforcement actions. Unfortunately, it doesn’t generate an easy referral link in which to view the data so I have not included the results.
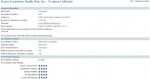
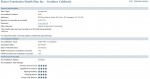
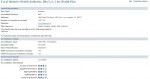
State of California Office of the Patient Advocate
Another state agency gathering data on health plans is the Office of the Patient Advocate. They collect data and issue a report card with a star rating on various patient care items such as maternity, cancer and mental health. Listed are the report cards for the type of insurance being offered through Covered California. Some plans offer both HMO and PPO plans, but I only included the link for the type of plan being offered through Covered California. The Medi-Cal ratings are included as another source of subjective data that might be used in determining how a plan might perform for individual health insurance. Not all health plans are obliged to release information or participate in the report. Hence, some of the plans will not be listed.
Report Cards
HMO Quality Ratings Summary 2013
PPO Quality Ratings Summary 2013
Medi-Cal Health Plan Quality Ratings
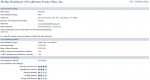
National Committee for Quality Assurance
The National Committee for Quality Assurance is a private nonprofit involved with improving health care quality. They rank health plans based on a standardized set of audit questions. NCQA Health Plan Report Cards not shown for a specific plan means the plan is either not part of NCQA or they are being scheduled for an evaluation. Because the audit is only at the company level, I’m not sure if they consider enforcement actions or if they conduct member surveys like Medicare. The insurance carriers below have NCQA report cards for the plan types shown.
- Anthem Blue Cross PPO, HMO, Medicare
- Blue Shield of California PPO, HMO, Medicare
- Health Net PPO, HMO, Medicare, Medi-Cal
- Kaiser HMO, Medicare
- L.A. Care Medi-Cal
- Molina Medi-Cal
- Western Health Advantage HMO
Hover cursor over image to see report card name and then click to enlarge image.
Medicare star ratings
Several of the plans included in Covered California offer Medicare Advantage health plans. Medicare Advantage plans are rated by the Centers for Medicare and Medicaid. Through an annual member survey and other data Medicare assigns a star rating to each plan. Medicare will place immediate sanction on a Medicare Advantage plan that is not meeting the requirements for customer service. The sanction immediately stops the insurer from marketing the plan or enrolling new members until the problems are corrected. Medicare Advantage plan comparison is difficult because they are issued by county and not state wide.
Fast Facts
The first place to look for information is on the company or plan website. Some websites provide more information than others and some are very poor when it comes to providing any statistical information. Valley Health Care and Ventura County Health Plan are two sites that are notable for their lack of information. While you can’t judge a book by its cover, I hope the limited design of the Valley Health Care and Ventura County Health Plan are not precursor to their customer service for new plan members.
- Alameda Alliance for Health
- Blue Cross of California
- Blue Shield
- Chinese Community Health Plan
- Contra Costa Health Plan
- Health Net
- Kaiser
- L.A. Care
- Molina
- Sharp
- Valley Health Plan
- Ventura County Health Plan
- Western Health Advantage
Customer Service
Since all the plans must offer all the same benefits, a large factor in choosing a health plan will center on their customer service. An organization that is not up to the task of handling questions, claims and other member services will create unhappy plan members. The model contract between Covered California and the insurers have minimum customer service requirements that must be met. Unfortunately, before Covered California starts measuring those customer service performance standards, consumers must rely on information already out in the public domain to make their decisions.