As President Biden’s American Rescue Plan nears completion, the federal stimulus package to address Covid-19 pandemic relief includes enhanced health insurance subsidies. Initially outlined, the federal subsidies may increase for many households in Covered California and also reach higher income levels. However, health insurance consumers in Covered California may miss out on the enhancement if they have not updated their consent for verification.
Consent for Verification Covered California
Once the American Rescue Plan is passed, signed into law, and begins to be implemented, Covered California will begin the process of reviewing active enrollments for their eligibility for the larger federal subsidies and other benefits of the relief package. In order for a consumer to take advantage of any health insurance subsidy enhancements they must have a current Consent for Verification.
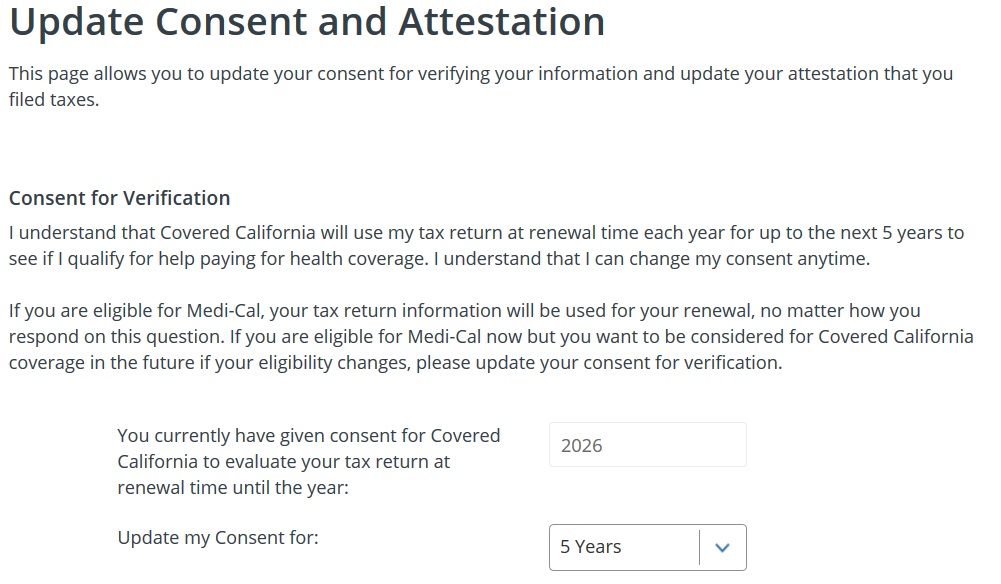
The Consent for Verification allows Covered California to reach out to federal and state databases and check eligibility conditions such as tax filing status, lawful presence, or other conditions such as Medicare eligibility. A consumer gives their consent for verification at the start of the application. They can then designate to have the consent renewed for up to five years.
No Consent, No Subsidy
Without the consent for verification, Covered California cannot forward any monthly Advance Premium Tax Credit subsidy to the health insurance carrier selected by the consumer. Many households, who may have forgotten to update their consent for verification during the Open Enrollment Period are shocked when they must pay the full premium amount of their health insurance. Updating the Consent for Verification restores the monthly subsidy.

You can check your Consent for Verification status by logging in to your Covered California account and scrolling down to the section “Account Information.” Click to expand the drop-down window and the Consent for Verification will be listed under Update Case Information section. If the date of consent is 2020, you will need to update it to at least 2021.
We need to let Covered California review all of the changes and enhancements to the health insurance subsidy before we know exactly how the changes will affect California consumers. California has expanded Medi-Cal along with the California Premium Assistance Subsidy. These programs rules need to be matched to any new subsidy and eligibility enhancements within the Covered California system. In other words, just because the new federal program states one thing, it may not apply to California or its implementation may be slightly different.


