Many Covered California consumers are confused over what seems to be contradicting statements of eligibility regarding the health insurance subsidy. The confusing statements are born out of Covered California’s assumption that consumers are experts, like they are, in the various subsidies and programs offered.

In addition to determining if an applicant is eligible for any health insurance premium assistance, the Covered California application is screening for four different programs.
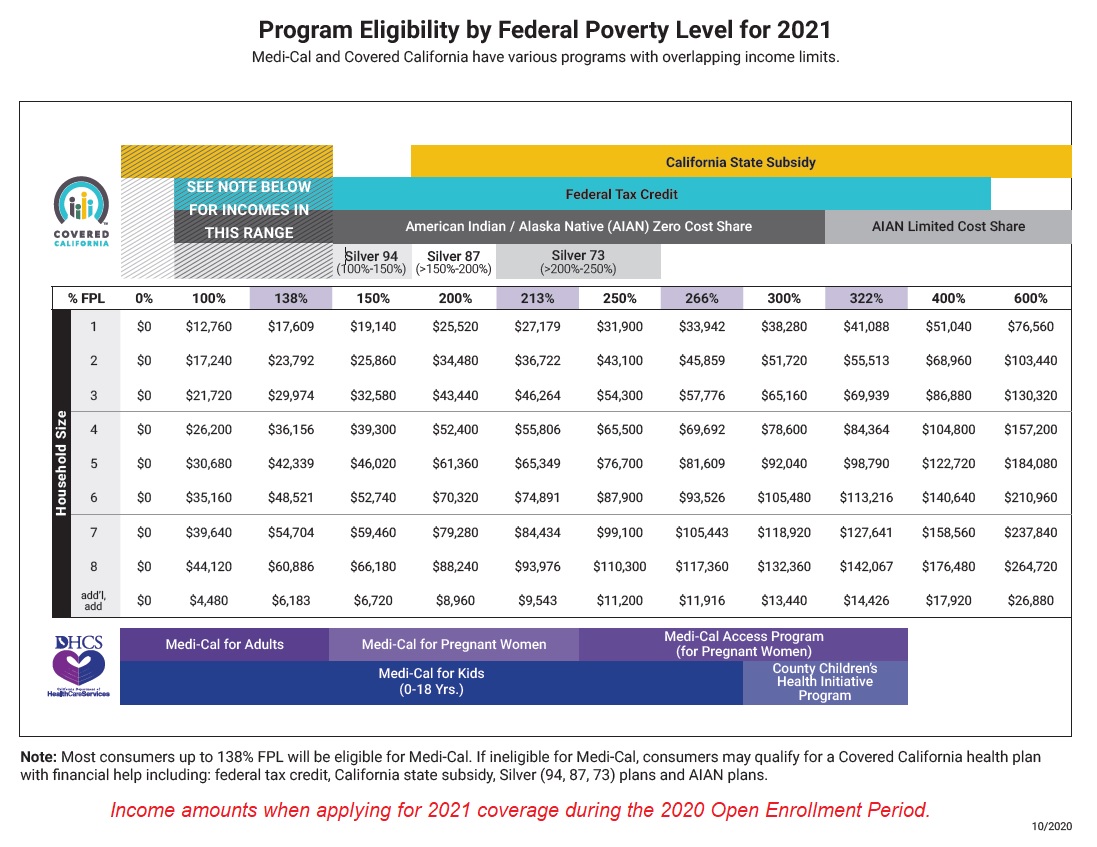
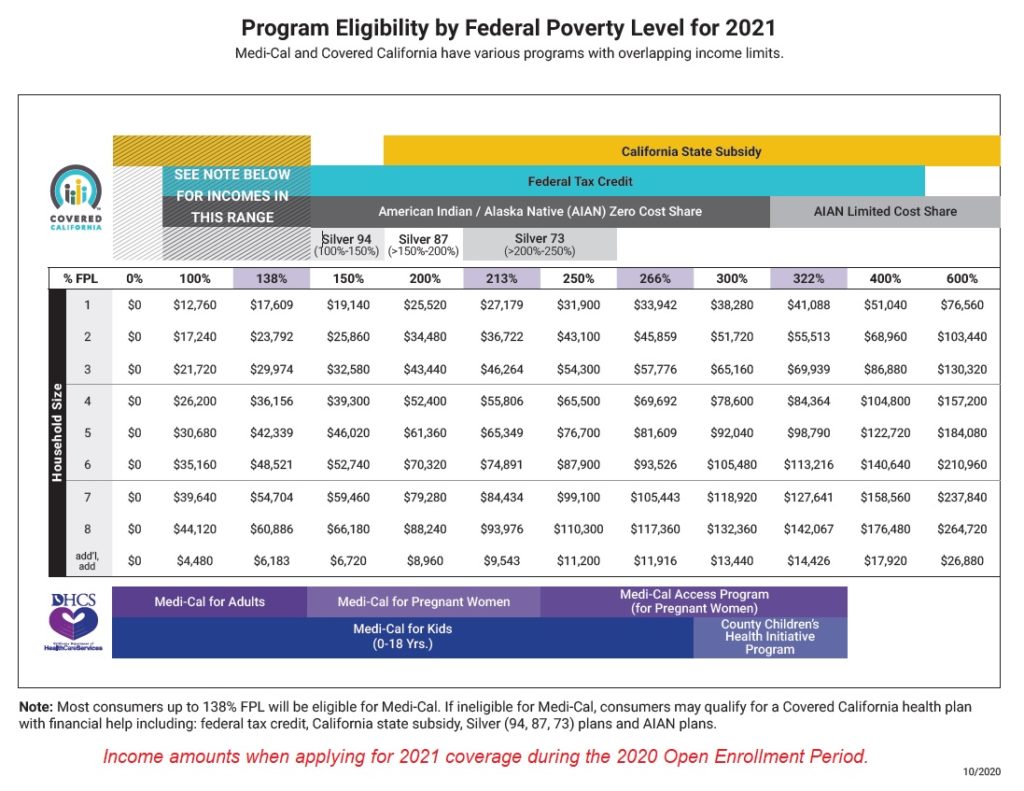
1. Federal Premium Tax Credit subsidy available to eligible consumers whose income is between 138 percent and 400 percent of the federal poverty level.
2. California Premium Subsidy available to eligible households whose income is between 200 percent and 600 percent of the federal poverty level.
3. Cost-sharing reduction (Enhanced Silver Plans 73, 87, and 94) targeted at household income between 138 percent and 250 percent of the federal poverty level.
4 Medi-Cal eligibility for adults whose income is below 138 percent of the federal poverty level and dependents, 18 years old and younger, where the household income is below 266 percent of the federal poverty level.
Covered California Eligibility Letter
You qualify for health and dental plans through Covered California. Your household qualifies for $xxx.xx per month in federal premium tax credit.
You also qualify for cost-sharing reductions.
You do not qualify for the California Premium Subsidy because you do not meet the income requirements.
You do not qualify for Medi-Cal because your income is above the limit.
The confusion lies in the statement that the consumer is not eligible for the California Premium Subsidy. The California Premium Subsidy program is completely separate from the federal Premium Tax Credit subsidy. You can be eligible for the federal subsidy but not the State subsidy. If your income is over 400 percent of the federal poverty level, you are not eligible for the federal Premium Tax Credit subsidy, but you may be eligible for the State subsidy.
The California Premium Subsidy will be reconciled on the taxpayer’s State income tax return, while the federal subsidy will be reported on the federal income tax return.
Some people are concerned that they are not eligible for the cost-sharing reductions erroneously assuming that those are the subsidies. The cost-sharing reduction plans Silver 73, 87, and 94 have reduced copayments, coinsurance, and maximum out-of-pocket amounts. Those reductions are in addition to any subsidy to lower the health insurance premium. You can only qualify for the cost-sharing reduction plans if your income falls into one of the percentile columns relative to the federal poverty level.
Many consumers are surprised to learn that Covered California is screening for Medi-Cal eligibility as they never applied for Medi-Cal. The Covered California application screens for Medi-Cal eligibility and many children are determined eligible for Medi-Cal and not the subsidies for a private health plan. Consequently, some letters sent to families will note that the adults are eligible for federal and/or State subsidy, while the children are in Medi-Cal.
See also: FAQ about the California Premium Subsidy.