You can’t hide your family status from Covered California. Are you pregnant?
In September of 2017 Covered California gave their health insurance and ACA subsidy eligibility application an extreme makeover. While all of the basic parts of the application are still present, the consumer can’t navigate to all the different sections like they use to under the old user interface. One significant change is that the consumer no longer has quick access to the household income summary. They can only gain access to it through the Report a Change function. Covered California has also added more pop-up window prompts for information that can cause and endless loop of frustration.
Household Income Summary Hidden From Consumers
New Covered California application does not give the consumer a way to view the household income summary unless you Report A Change to Income under Special Enrollment Period.
Before the CalHEERS 17.9 was deployed a consumer or agent could easily review the household income information. This was convenient because many times a consumer had a question about how they entered the household income, but didn’t necessary want to change it. For example, did the consumer enter their spouse’s income or the modest invest income correctly? What is the total household income being used to calculate the Advance Premium Tax Credit? Sometimes, with a quick review, nothing needs to be changed.
Under the new account information display, the only way to review the household income is to Report A Change. Reporting a change triggers the screens for a Special Enrollment Period (SEP) application and selecting a qualifying event. If you work with the Covered California application all the time, it’s easy to back out of the SEP function without making any changes. But if you are not familiar with new screens and flow of the application, some consumers may end up submitting a change they don’t want to when all they wanted to do was review their income data.
Special Enrollment To Report Change To Income
The SEP screen is not necessarily intuitive when you do actually want to report a change to income. Reporting a change of income does trigger a SEP because a new income amount may put some household members in Medi-Cal, push the household out of the Enhanced Silver 73, 87, or 94 range, or make them ineligible for the tax credit subsidy altogether. If a mistake is made which inadvertently makes some household members eligible for Medi-Cal, there is very little Covered California can do. At that point, it is in the hands of the county Medi-Cal office and all income verifications, even to correct a mistake, must go through Medi-Cal.
However, I did encounter one Medi-Cal eligibility determination that Covered California was able to correct. I had a family who already had a household income over 266% of the federal poverty line and their two dependents were not eligible for Medi-Cal. Under the new Covered California application, I was reporting a change of income for a higher amount that was over 400% of the federal poverty level. An income over 400% means the household is not eligible for the monthly premium tax credit subsidy.
When I submitted the income change report to Covered California the system determined the two dependents, who are under 18 years old, plus the 23 year old daughter, as Medi-Cal eligible. Fortunately, Covered California was able to flip an internal switch from an application seeking assistance to household not seeking the monthly subsidy. This made all the household members eligible for private health insurance through Covered California. No one was able to explain why three of the household members were made Medi-Cal eligible when clearly, based on income, they were not.
Is Anyone Pregnant?
Another annoying change Covered California made was adding little pop-up windows asking for more information called One More Thing. After submitting a change to the income, Covered California wants to know if anyone is pregnant. The only way to get around this is to select the Edit button and select Nobody from the household member selection. The first time I did this it must not have registered because I got placed back into the pregnancy loop again. Once the Nobody selection was logged, I was able to move forward. Part of the rational for the pregnancy test is to see if the pregnant household member might be eligible for Medi-Cal benefits.
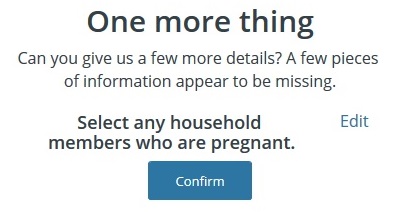
Covered California will ask if anyone is pregnant in the household. You must select Edit and either the pregnant household member or Nobody.

Selecting Nobody will allow you to continue to submit the change report to Covered California.
Another One More Thing window asks for additional information about the household members. Anytime you report a change the Covered California system looks at fields you may have accessed or might be part of the change. You may get a page where you have to state the reason for the change to the household member that you never made. Where possible, I select Other, or most appropriate reason, as the reason and today’s date, then move to the next household member and reason. This is no different from the previous Covered California explanation for the change submission, it just looks different. Previously, Covered California was not evaluating whether the selected reason was valid.
This pop up menu may appear when you are submitting a change report.
Check Box After Scrolling
Finally, when you get to the last page to submit the changes, you have to check mark a box indicating that you understand the legalese of enrolling through Covered California. No matter how hard you try you cannot check mark this box. The system will allow you to check the box once you have scrolled completely through the in-page window that has all the text. They want to make sure you have read the fine print. The instructions tell you to scroll all the way to the bottom. Silly me, I though they meant scroll all the way down to the bottom of the page, not the window.

The Manage Application Menu will display different options depending on where the consumer is in the application.
Outside of open enrollment, the Covered California system assumes you want to report a change. The bulk of the home screen is devoted to navigating the consumer through reporting a change. Scroll all the way down to the bottom of the page to find Manage My Application. A list of available actions will be displayed. Selecting View enrollment summary will get you to basics of the application, with the exception of the income summary. The Manage My Application choices will change depending where you are at with either reporting a change or selecting a new health plan after a change has been reported.
For all the changes Covered California has said they made to their application see
Major Covered California Online Application Update for 2018 Open Enrollment


