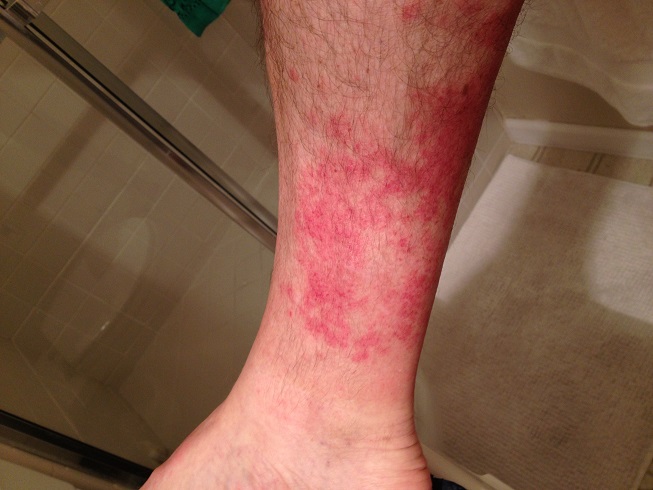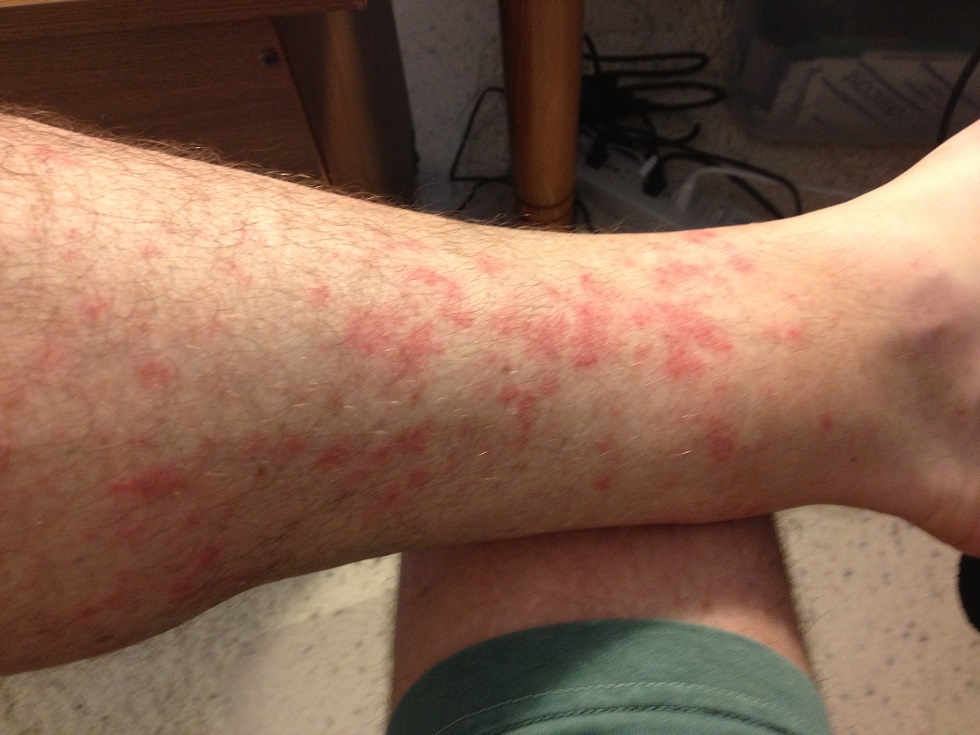
It was after a particularly long hike up Palm Canyon in Palm Springs that I first noticed the rash on my legs. Since I was 6 hours from home and had planned my little hiking adventure months in advance, I wasn’t going to let a little rash stop me. (Click on photos to enlarge thumbnails)
Hiker’s rash was a surprise
The rash was concentrated below my knee so I figured it had something to do with laundry detergent or heat. I have long suffered from a particularly vexing itching condition on my neck and arms, which never produces a rash, so I always have 3 or 4 tubes of hydrocortisone cream scattered between the house and car. To combat the mild itch in Palm Springs I just slathered my legs with hydrocortisone cream.
Maybe psoriasis?
I didn’t have another recurrence of the rash until the spring of 2012. The rash was
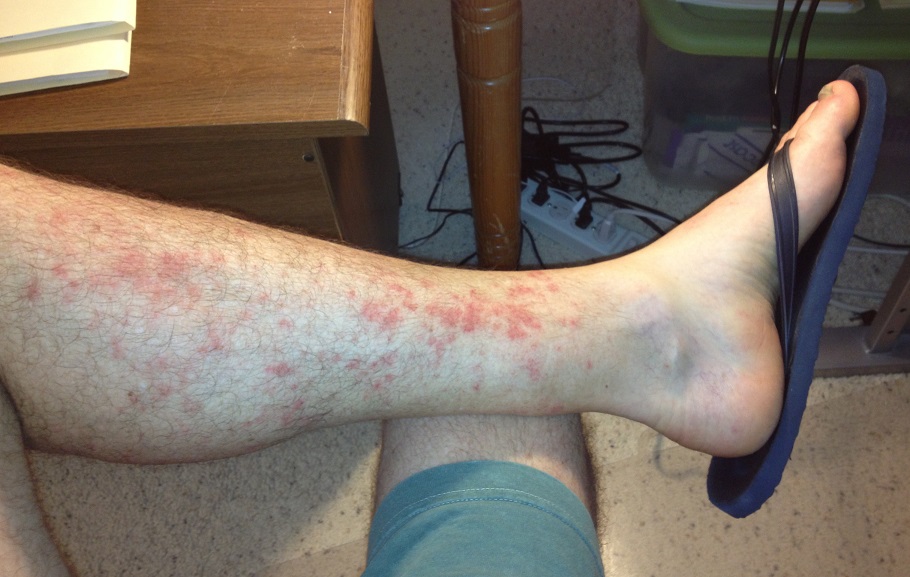
again primarily between my knee and ankle on my legs. This time I did go see a doctor and he prescribed a stronger steroid cream, Triamcinolone Acetonide, but it didn’t really seem to make any difference in the severity or duration. Another leg rash in the summer convinced me I might have psoriasis so I bought some drug store medication that contained 3% Salicylic Acid. The psoriasis medication was no more effective than the steroid cream.
Had to be shingles
After the last episode I attached an M.D. after my name and diagnosed myself has suffering from shingles. The symptoms were almost classic: late 40 year old male who had chicken pox as a child and a rash that was identical to the pictures of shingles. The only problem was that the rash wasn’t on my abdomen, was only mildly itchy, and only minor pain associated with it.
I watched it grow on my legs
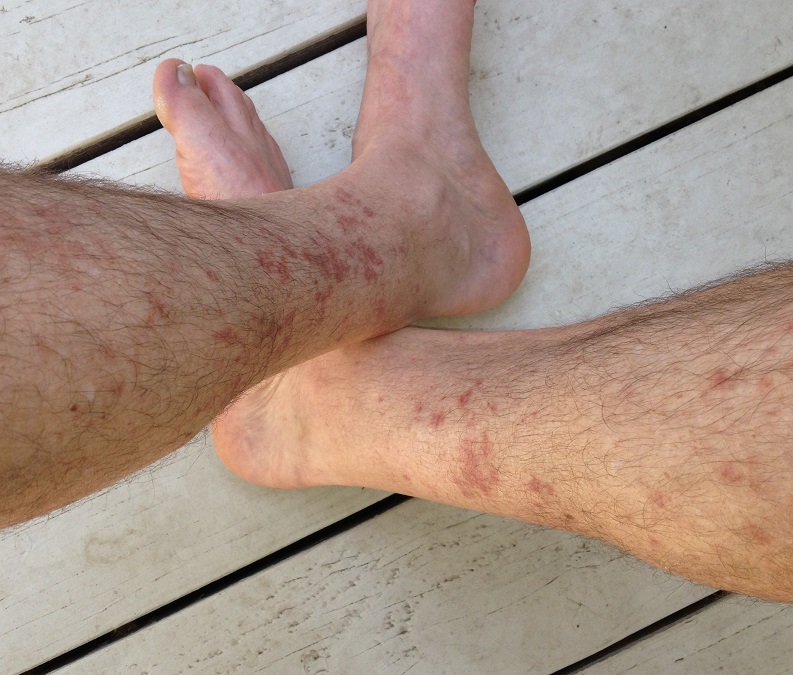
May 2, 2013: my first hike of the year wearing shorts. On a warm spring day I took a 4 hour hike on the Auburn Quarry trail. Within a couple hours of hiking I noticed some redness on my legs below the knee. By that evening, the angry red rash had broken out on my legs. The worst of the rash was on the inside of my legs and calf, the area least likely to brush up against weeds or be exposed to the sun. I named it hiker’s rash and apparently I am not the first person to do so. A quick search for “hiker’s rash” turned up lots of hits.
Stuffy, bloody nose after hiking
October 15, 2015, addition; Over the last year I’ve experienced another odd ailment after long hikes – a stuffy and bloody nose. Usually the day after a hike of three to six hours in length covering five to eight miles, my nose becomes stuffed up with blood. I am not talking large quantities, but when I blow my nose (I apologize for the descriptions), there is dried blood and sometimes some fresh blood. This is not dripping down my face. It is more like a sinus congestion with little micro-bleeds inside my nasal passages.
The stuffy bloody nose occurs whether I have developed the hiker’s rash or not. But it does last for about the same duration of one to three days. It is almost as if the malady that affects my lower legs is now, or always has been, also in my nose or sinuses. Most of my hikes have been at no higher than about 500 feet in elevation around the American River canyons northeast of Sacramento. The humidity is low, typical of California summer and autumn, and their is no abundance of dust or pollen. It even occurred when I went hiking back in Massachusetts at the end of August. From my perspective, this is not an environmental condition so much as a physiological response similar to hiker’s rash.
What were the triggers?
Up until this point I had attributed the mild cases of the rash to brushing up against weeds and plants as I was mountain biking on the trails around Folsom Lake. But after carefully watching the rash develop after the last hike, I am certain the trigger has to do with physical exercise, either biking or hiking. I would like to say the sun is a contributing factor, but my rash has developed even while wearing long pants.
### Update: August 2, 2013 ###
FDA Warns of Rare Skin Reactions to Acetaminophen
The widely used painkiller acetaminophen, best known as Tylenol, can cause rare but serious skin reactions and a warning about this danger will be added to product labels, the U.S. Food and Drug Administration said Thursday.
The severity of the reactions they describe are beyond what I and most people who have commented on this post have experience. However, it might have a bearing for some people and if this common over-the-counter pain medicine can create a skin rash, some of us might also be experiencing adverse effects from other medications we are taking.
### Original post continues ###
Short walks, no problems
It was just a week earlier that we took a short hike at Folsom, wearing shorts and I didn’t break out in a rash. Although, it hindsight, I did develop some small red blotches that I thought possibly came from stickers on the Folsom lake hike. Perhaps those little red bumps were a precursor to the more full blown episode.
Running doesn’t cause break out
On a good weekend I will run 4 to 5 miles at the lake each morning and ride my bike in the afternoon. None of this activity along with regular yard work triggers the rash. It is only prolonged hiking of two or more hours that seems to be the initiator for my hiker’s rash. The only other physiological symptom is after several hours of hiking my fingers get slightly swollen.
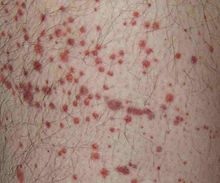
Clusters of blood blisters
The red blotchy rash is like little clusters with little pin pricks of red 8 to 10 millimeters across. The cluster will have 4 or 5 red dots that may or may not develop into blisters. A short duration rash will gradually fade away in a week. Some outbreaks have lasted weeks with some of the clusters growing and others blistering
Experimental cure
At this point I have decided to become a human Guinean pig and treat one leg with hydrocortisone cream and let the other heal naturally. I didn’t expect that the steroid cream to have any pronounced effect and it didn’t. Some of my rashes may have been from some other ailment like psoriasis or shingles. Because each episode can be a little different in intensity, severity and duration, I have not ruled anything out.
All I am certain about is that-
- The hiking rashes started in my late forties.
- Concentrated between knee and ankle.
- Will last one to four weeks.
- Develop after hiking at least for three hours.
- Only time seems to make the rash fade.
Tattoo Rash

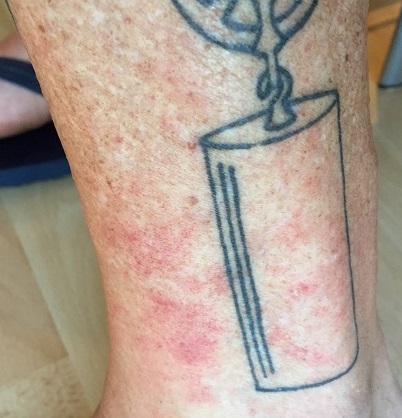
On September 23rd, 2017, I got a tattoo on my right calf. The tattoo guy shaved the area where the tattoo was to be placed. On September 29, 2017, one week later, I went for a dusty two hour hike. Before I went I had put ointment on my tattoo area (as advised in the after-care instructions) and I put on 30 SPF sun screen on the tattoo.
After the hike, only the portion that had been shaved for the tattoo had the rash. I have a similar tattoo on my left calf that I got months earlier and it was not affected by the hike at all. This was the first time I ever had a rash associated with a tattoo.
May 23, 2020 – I had not developed the hiker’s rash for a couple years. On a nice Saturday morning I went for a 12 mile hike out at Folsom lake with socks and light weight gators. I barely broke a sweat. Later that afternoon the rash developed again under and around my new tattoos. My ankles, where the rash predominated, were completely covered, no sun, no weeds, no dust. The presence of tattoos seems to have no affect at all. It neither makes the rash worse or prevents it.
It seems as if more women have commented about getting the hiker’s rash than men. Women have a higher probability of shaving their legs on a regular basis than men do. I’m wondering if leg shaving is partly the cause to the hiker’s rash in some people. It doesn’t account for all the incidents of hiker’s rash. I never shaved my legs and yet I still got the rash.
FDA Approves Mirvaso
In an email from healthfinder.gov they reported FDA Approves 1st Topical Gel to Ease Redness of Rosacea.
Rosacea is a chronic inflammatory and vascular ailment that affects the face, causing redness and visible blood vessels as blemishes appear on the forehead, nose and cheeks. The condition is most common in people over 30 and is thought to affect about 16 million Americans, according to the news release.
According to the company, Mirvaso is thought to work by constricting otherwise dilated facial blood vessels, cutting down on the appearance of redness. The gel is applied once a day to the forehead, chin, nose and cheeks, Galderma said. It will be available in pharmacies in September.
Sound familiar, inflammation of the vascular system near the skin. Sounds like hiker’s rash or vasculitis. While the standard hiker’s rash seems to fade away after 3 days, I know some people suffer longer. I sent a tweet to @kraussderm, Krauss Dermatology, to get their opinion of Mirvaso as a potential treatment for hiker’s rash. I’ll post any update if and when I learn anything.
If you have any suggestions for avoiding hiker’s rash or lessen an episode, please pass them along. I know that I am not the only one who suffers from this condition.
**Update May 27, 2013
On week of May 19th, I went on 3 hikes that were each over four hours long. The first two hikes were along the South Fork American River Trail. After neither these hikes did I develop a rash. For the most part, there was always a trail, that while very dusty, was free of weeds. Although I did travel occasionally off trail to take a picture, it was very minimal.
On Sunday May 26 we took a long hike across the Table Mountain Preserve. The short distance to get to Phantom Falls was to blaze a trail across the mesa through the weeks. I would estimate that at least 2 of the 5 hours hiking was actually spent walking through dry grass and weeds. By the fourth hour on a stretch that was all trail, my calves were burning like I had a sun burn. But I knew it couldn’t be a sun burn since on the two previous hikes, during the same time of day and heat, I barely got a tan.
By the time I finally took a shower and washed the dirt off, the skin rash was bright red and covered from right below the knee to the top of the ankle. I was wearing short and ankle high socks. While I am no doctor, I am going to say that I am having some sort of allergic reaction to the combination of the weeds, hiking, sun and dust. When present in the right combination, the hiker’s rash breaks out on my lower legs.
Two hikes, two results
On September 26th I took a 10 mile hike that was completed in approximately two hours and forty-five minutes. The terrain was flat and the weather dry and in the mid-70 degrees. No rash developed. Two day later on September 28th I walked along the Dish Trail at Stanford University. It was warm, mid-80’s, and there was 200 foot elevation gain that was we walked up three different times. At the end of the six mile hike over about three hours, I developed Hiker’s Rash. I was wearing essentially the same shoes, socks, shorts and shirts as the previous hike. I can only attribute the rash to ascending or descending the trail.
I actually hiked faster and harder on my Paradise Lake hike than at Stanford. But there was no extra exertion of climbing hills or the jarring hit of my foot on the descent of trail up in Paradise. Perhaps the pressure created from either climbing or descending in elevation causes the blood vessels to break and create the rash.
***Update June 24, 2013***
Leukocytoclastic Vasculitis
I happened to see a Twitter post from a dermatologist asking for questions that the office might help with. I sent a link of this blog post to Krauss Dermatology (@KraussDerm) and received a response alluded to by several people including a comment on this blog post:
@Insuremekevin It could be exercised induced leukocytic vasculitis. A biopsy when the rash is present is necessary to make the diagnosis.
While I haven’t found the exact term leukocytic vasculitis, there are many references to leukocytoclastic vasculitis. Leukocytoclastic stands for the destruction of or by white blood cells and vaculitis is the inflammation of blood vessels. (Not having a medical background I need this stuff spelled out for me in plain english).
Hypersensitivity vasculitis may be the closest reference I have found relating to exercised induced leukocytoclastic vasculitis. The article doesn’t say much, but it has a good picture.
This discussion on wiseGeek about leukocytoclastic vasculitis offers more description.
Donna Hicks details her bout of leukocytoclastic vasculitis on Yahoo News. Her medical became serious enough to seek medical attention from professionals who continually mid-diagnosed her. A common thread in all the descriptions is the potential for internal organs to be afflicted with inflammation and destruction of blood vessels. Some of the references mention that the episodes of hikers rash as we have come to call it, will fade away and be recurring.
Is episodic hiker’s rash a precursor to more serious out breaks either on the skin or internally? My worst episode was my first two years ago with a growing and spreading rash. I will admit that I was hiking five days straight down in Palm Springs and that may have been a contributing factor to the severity of my outbreak. Since then, my hiker’s rash outbreaks have been less intense and seem to fade out much quicker, usually within 3 days.
I am going to err on the side of optimism from the tone and experience of the comments to this post. Our hiker’s rash is elusive in its trigger points, but isn’t a dire medical condition that necessitates immediate medical attention. Of course, everyone is different and should seek the medical treatment appropriate for the situation.
Associated Blog Post: Uncontrollable Itching on Neck, Arms from Stress and Anxiety
_________________________________________________________________
Additional Links posted on July 31, 2013
The number of comments and request for answers prompted me to post more links regarding this skin condition. Something is causing blood vessels and capillaries to swell and burst under our skin. Maybe this is just a condition of getting older or perhaps indicators of a more serious disease. As is my nature, I need answers, preferably scientific answers, to make sense of this queer hiker rash thing.
I am not a physician. However, from the material I have come across there seems to be an auto-immune response happening in our legs. There are a variety of triggers that can cause this vasculitis from heat, cold, exercise, pollen, plants, prescription drug and possibly as a manifestation of an associated disease within the body.
There are hundreds of links to a variety of skin conditions that could produce the purpura rash like symptoms. I have chose to post just a few with an accompanying definition. If there was additional information that might link to the overall condition, I included that as well. All of these links are from Wikipedia with the exception of the Nettle Rash from the National Health Service, U.K.
Vasculitis: a group of disorders that destroy blood vessels by inflammation, primarily due to luekocyte migration and resultant damage.
Luekocyte: White blood cells, or leukocytes (also spelled “leucocytes”) are cells of the immune system involved in defending the body against bothinfectious disease and foreign materials. Fivedifferent and diverse types of leukocytes exist, but they are all produced and derived from a multipotent cell in the bone marrow known as a hematopoietic stem cell.
Basophil granulocyte: one of five types of luekocytes in the blood. Basophils appear in many specific kinds of inflammatory reactions, particularly those that cause allergic symptoms. Basophils contain anticoagulant heparin, which prevents blood from clotting too quickly. They also contain the vasodilator histamine, which promotes blood flow to tissues. They can be found in unusually high numbers at sites of ectoparasite infection, e.g., ticks. Like eosinophils, basophils play a role in both parasitic infections and allergies. They are found in tissues where allergic reactions are occurring and probably contribute to the severity of these reactions.
Histamine increases the permeability of the capillaries to white blood cells and some proteins, to allow them to engage pathogens in the infected tissues. Histamine is an organic nitrogen compound involved in local immune responses as well as regulating physiological function in the gut and acting as aneurotransmitter.[2] Histamine triggers the inflammatory response. As part of an immune response to foreign pathogens, histamine is produced bybasophils and by mast cells found in nearby connective tissues.
Cutaneous small-vessel vasculitis: inflammation of small blood vessels (usually post-capillary venules in the dermis), characterized by palpable purpura. It is the most common vasculitis seen in clinical practice. Leukocytoclasis refers to the damage caused by nuclear debris from infiltrating neutrophils in and around the vessels.
Purpura: is the appearance of red or purple discolorations on the skin that do not blanch on applying pressure. They are caused by bleeding underneath the skin usually secondary to vasculitis or dietary deficiency of vitamin C (scurvy). Purpura measure 0.3–1 cm (3–10 mm), whereas petechiae measure less than 3 mm, and ecchymoses greater than 1 cm.
Petechia: red or purple spot on the body, caused by a minor hemorrhage (brokencapillary blood vessels). The most common cause of petechiae is through physical trauma such as a hard bout of coughing, vomiting or crying, which can result in facial petechiae, especially around the eyes. Petechiae in this instance are harmless and usually disappear within a few days. Petechiae may be a sign ofthrombocytopenia (low platelet counts) when platelet function is inhibited (e.g., as a side effect of medications or during certain infections), or in clotting factor deficiencies.[1] They may also occur when excessive pressure is applied to tissue (e.g., when a tourniquet is applied to an extremity or with excessive coughing or vomiting).
They can be interpreted as vasculitis, an inflammation of the blood vessels, which requires immediate treatment to prevent permanent damage. Some malignancies can also cause petechiae to appear. Petechiae should be investigated by a doctor to rule out the more dangerous conditions. Dermatologists can be the most helpful specialists in these conditions because they can more easily identify if the condition is petechiae or some similar looking but less worrisome rash.
Urticarial vasculitis: a skin condition characterized by fixed urticarial lesions that appear histologically as a vasculitis. A rare autoimmune disease characterised by recurrent urticaria (nettle rash), first described in the 1970s. There is no defined paradigm for the syndrome aetiology and severity in progression. Diagnosis is confirmed with the identification of at least two conditions from: venulitis on skin biopsy, arthritis, ocular inflammation, abdominal pain or positive C1q antibodies to immune complexes.
Nettle Rash – Hives – Urticaria: Urticaria (also known as hives, welts or nettle rash) is a raised, itchy rash that appears on the skin. The rash can be limited to one part of the body or spread across large areas of the body. The affected area of skin will typically change within 24 hours, and usually the rash will settle within a few days.
Urticaria happens when a trigger causes high levels of histamine and other chemical messengers to be released in the skin. These substances cause the blood vessels in the affected area of skin to open up (often causing redness or pinkness) and become leaky. This extra fluid in the tissues causes swelling and sometimes itchiness.
Histamine is released for a wide range of reasons, including:
- an allergic reaction to substances such as latex
- exposure to cold or heat
- infection
- the direct effect of certain chemicals which can be found in some types of food and medications, such as non-steroidal anti-inflammatory drugs (NSAIDs)
Henoch-Schonlein purpura: HSP is a systemic vasculitis (inflammation of blood vessels) and is characterized by deposition of immune
complexes containing the antibody IgA; the exact cause for this phenomenon is unknown. It usually resolves within several weeks and requires no treatment apart from symptom control, but may relapse in a third of the cases and cause irreversible kidney damage in about one in a hundred cases.
HSP effects the skin and other organs that most commonly affects children. In the skin, the disease causes palpable purpura (small hemorrhages); often with joint and abdominal pain.
Henoch–Schönlein purpura is a small-vessel vasculitis in which complexes of immunoglobulin A (IgA) and complement component 3 (C3) are deposited on arterioles, capillaries, and venules. As with IgA nephropathy, serum levels of IgA are high in HSP and there are identical findings on renal biopsy; however, IgA nephropathy has a predilection for young adults while HSP is more predominant among children.
Hiker’s Rash Update September 23, 2013
This latest update was brought to us by “Kevin” who posted the links to the following article.
Exercise-induced urticarial vasculitis as a paraneoplastic manifestation of cystic teratoma
Urticarial Vasculitis: A rare autoimmune disease characterized by recurrent urticaria (nettle rash), first described in the 1970s.
Paraneoplastic manifestation: disease or symptom that is the consequence of the presence of cancer in the body, but is not due to the local presence of cancer cells.
Cystic teratoma: encapsulated tumor with tissue or organ components resembling normal derivatives of more than one germ layer.
Essesntially, this 42 year old gentlemen in the article would break out in a rash on his lower extremities after vigorous exercise. Like a typical hiker’s rash it would fade after 3 days. The doctors performed lots of tests and could find no problems. They then decided to try and create the rash through monitored exercise in a laboratory.
Within 5–6 h after exercise challenge, urticarial lesions developed on the patient’s legs and started to disappear at 72 h, leaving slight pigmentation. Skin biopsy was carried out at 24 h, and histology was again indicative of leucocytoclastic vasculitis. The investigations were completed with abdominal ultrasound, which was normal, and a chest X-ray, which showed a tiny widening of the superior mediastinum. Therefore, the patient underwent a chest computed tomography scan, which showed a cystic mass in the anterior superior mediastinum. A chest MRI scan revealed that this mass was very well demarcated and had the imaging features of a cystic teratoma. – F. Di Stefano, S. Siriruttanapruk and M. Di Gioacchino
After surgically removing the cyst the gentleman was able to return to normal exercising with no recurrence of the rash.
We believe this is the first report of UV as a paraneoplastic manifestation which is triggered by physical exercise. The exact pathogenesis of the association of UV with malignancy is unclear. It is thought that tumour-associated immune complexes may give rise to complement fixation in the vessel wall and subsequent development of an inflammatory process [6]. In exercise-induced UV it has been shown that mast cells are the first to be involved, with the activation and subsequent release of proinflammatory mediators.. F. Di Stefano, S. Siriruttanapruk and M. Di Gioacchino
Conclusions
If you have the hiker’s rash that consistently recurs then it might be wise to have some imaging done after you show this article to your physician. This particular case substantiates one commentator’s hypothesis of an auto-immune response. The unknown is if the auto-immune response is from an external allergen like grasses or from an internal tumor.
July 2, 2014 Autoimmune response
While this article from the Washington Post is not about hiker’s rash, it does involve the body’s autoimmune response. The article, A fever gripped a woman every afternoon, only to slide back to normal while she slept, chronicles one woman’s journey to get a diagnosis for her daily fever spikes.
But the real surprise lay in her right ovary. Doctors found evidence of a rare autoimmune disorder that appeared to be giant cell arteritis. Also called temporal arteritis, it is a vascular condition in which the linings of the body’s large arteries, including those leading to the heart, become inflamed, causing them to thicken and narrow, resulting in decreased blood flow.
While her problem actually turns out to be another disease called Takayasu’s arteritis, the same inflammation was occurring. Bottom line, our bodies to weird things in response to perceived internal and external sources of threat.
Sarcoidosis immune reaction
An individual posted a comment relating how she had been diagnosed with Sarcoidosis which triggers a response in the immune system from an infection or other trigger like an antigen. (https://en.wikipedia.org/wiki/Sarcoidosis)
I was diagnosed with an autoimmune disease Sarcoidosis around 7 years ago and this started happening to me a couple years later. I don’t hike, but everytime I do a lot of walking it does this. It also does it when I drink alcohol, but not as bad. I’m 38 and female. – MJ
While most references cite an affliction with the lungs because of Sarcoidosis, the titerature also discusses a variety of different type of rashes that may develop on the skin because of the immune response.
Wikipedia article Sarcoidosis
Skin
Main article: Cutaneous manifestations of sarcoidosisSarcoidosis involves the skin in between 9 and 37% of persons and is more common in African Americans than in their white counterparts.[2] The skin is the second most commonly affected organ, after the lungs.[21] The most common lesions are erythema nodosum, plaques, maculopapular eruptions, subcutaneous nodules, and lupus pernio.[21] Treatment is not required, since the lesions usually resolve spontaneously in two to four weeks. Although it may be disfiguring, cutaneous sarcoidosis rarely causes major problems.[2][22][23] Sarcoidosis of the scalp presents with diffuse or patchy hair loss.[24][25]
The strong similarity between Hiker’s Rash and Sarcoidosis is that immune reaction seems to clear up on their own without medical intervention. I am not suggesting that everyone who develops Hiker’s Rash has Sarcoidosis, but there is obviously a strong link between episodic manifestations of symptoms of how both Hiker’s Rash and Sarcoidosis appear and then clear up over a period of time.