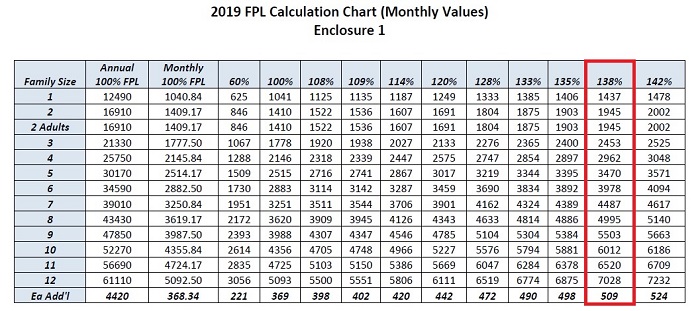
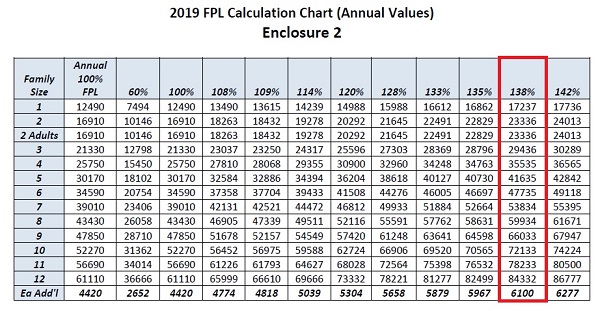
California Department of Health Care Services has updated the income levels for the various Medi-Cal programs they administer for 2019. They are based on the federal poverty level income numbers published by the federal government. The benchmark 100% federal poverty level income for a single adult increased 3% from $12,140 in 2018 to $12,490 for 2019. The all important Covered California premium tax credit eligibility income (138% of the FPL) for a single adult increased from $16,754 for 2018 to $17,237 in 2019. This means a single adult now has to have an annual Modified Adjusted Gross Income (MAGI) of $17,237 to be eligible for Covered California if they apply for health insurance in 2019.
Federal Poverty Level Income Increased 3% For 2019
Covered California and Medi-Cal have indicated that if an individual or family applied for health insurance in 2018, for the 2019 year, their estimated MAGI would be subject to 2018 FPLs. This also applies to consumers who were automatically renewed for 2019. Individuals and families applying for health coverage in 2019 with a qualifying event for a Special Enrollment Period will have their MAGI compared to the 2019 FPLs.
Will Covered California Consumers Be Subject To Higher FPL Income Levels?
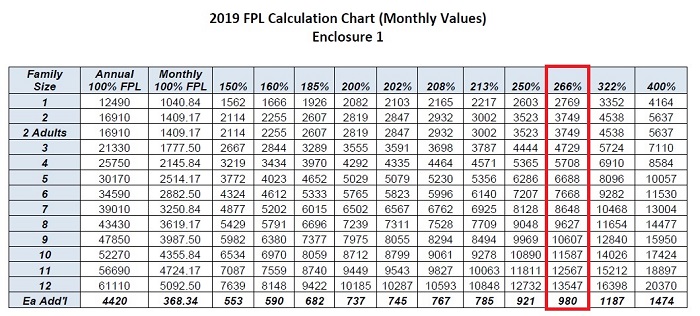
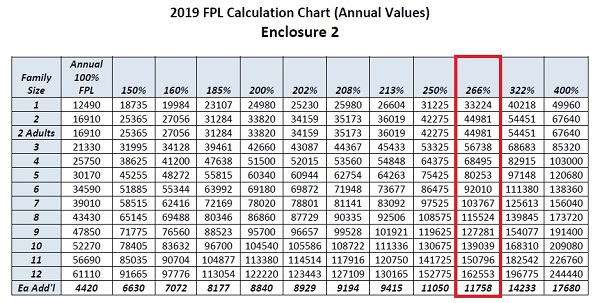
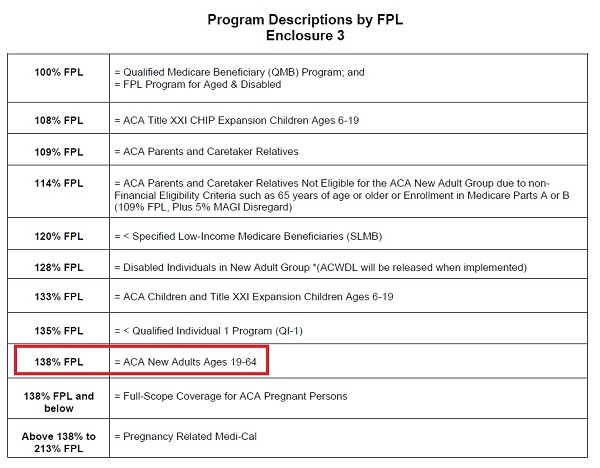
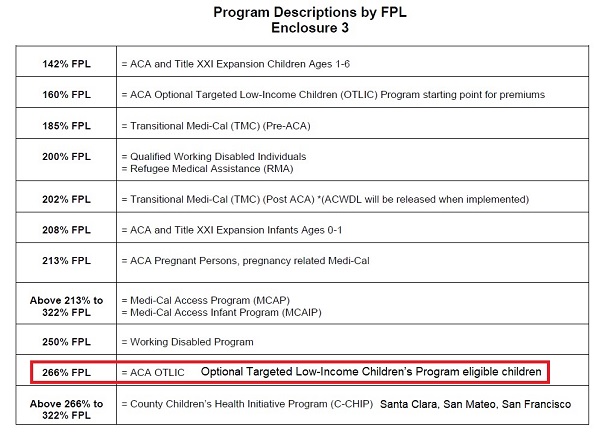
What is somewhat of a gray area is if an existing Covered California consumer makes a change to their income, which falls under the SEP guidelines of the Covered California online application, will the new income be subject to the 2018 or 2019 FPLs? This could be hazardous for some people with children. Household income below 266% of the FPL has dependent children automatically enrolled in Medi-Cal and not eligible for Covered California and a private health plan with the monthly premium tax credit assistance. In 2018, for a family of four, 266% FPL was $66,766. In 2019 it was raised to $68,495. If the family income at renewal time was $66,800, all members of the 4-person household were Covered California eligible. In 2019, if the same family raises the income to $68,000, that is under the 2019 266% of the FPL and MAY automatically make the children Medi-Cal eligible.
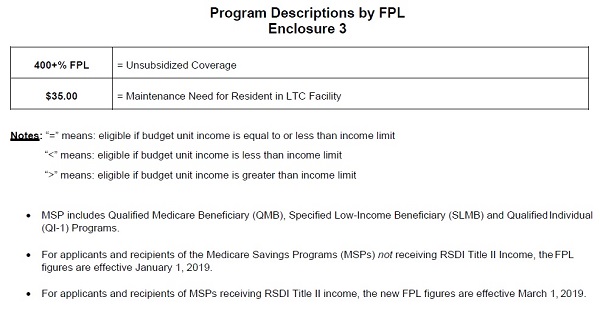
The Medi-Cal FPL income levels also apply to programs such as pregnancy related Medi-Cal, caretakes of disabled individuals, and dual eligible Medicare and Medi-Cal beneficiaries.
Department of Health Care Services sent out a notice to their County Welfare Directors about the 2019 FPLs and Covered California updates. From the notification, if a consumer applied for health insurance in 2018, but did not bind the coverage or failed to make premium payments, they would be subject to the 2019 FPLs
Due to delays in implementing these FPLs in the California Healthcare Eligibility, Enrollment, and Retention System (CalHEERS), DHCS has initiated a Change Request for the CalHEERS system to update the annual FPL amounts automatically. However, DHCS will still need to send a notice to the beneficiaries potentially impacted by the change to inform them of the FPL increase and that they may request a redetermination. The Centers for Medicare and Medicaid Services has decided that there will be no reimbursement for premiums paid. The notice will state that no premium reimbursements will be available. Therefore, counties shall retroactively change eligibility only for those Optional Targeted Low-Income Children’s Program eligible children, Advance Premium Tax Credit eligible individuals who did not enroll in a plan or did not pay a premium, and individuals who are eligible only for the Medi-Cal programs with a Share-of-Cost in the same month. – ACWD Letter 18-03