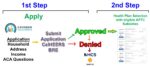
I have seen where the information all looks correct, but Medi-Cal never resubmitted the application. Medi-Cal changes their database and that of Covered California. However, if those changes are not properly processed through CalHEERS, your results may not be correct.