
Blue Shield of California states they can’t stop doctors from discriminating against Covered California members.
Since the beginning of Covered California, many individuals and families have complained that some doctors refuse to accept health insurance purchased through Covered California. Most health insurance companies have stated that contracted network doctors can’t refuse to see Covered California members. However, Blue Shield of California seems to have changed their position on doctors refusing service. They are now stating, as of November 7th, that doctors can discriminate against individuals and families who have Covered California plans.
Blue Shield Doctors Discriminating Against Covered California
Even when an individual is denied service or has his or her Covered California health plan rejected, most consumers are reluctant to file a complaint. They are afraid their complaint will become known to the doctor and then the doctor will refuse to see them even on a cash-payment basis. In October, I did have one client who wanted to push the issue as he felt he was being unfairly discriminated against.
In-Network Doctors Deny Covered California Members Appointments
One doctor’s office openly told him that they would accept a Blue Shield individual and family plan purchased off-exchange, directly from Blue Shield, but not through Covered California. Another doctor had it prominently displayed on his website that he did not accept Blue Shield Covered California plans. Both of the doctors in the Bay Area were listed on the Blue Shield Find a Provider online directory list as being in-network. My client, who was applying for coverage through Covered California under a Special Enrollment Period, specifically chose Blue Shield because these providers were listed as in-network.

Some doctors openly announce their discrimination against Covered California members with Blue Shield plans, even though they are listed as in-network with Blue Shield.
Blue Shield use to educate doctors
Back in 2015, I was told that Blue Shield took the issue of doctors not accepting Covered California plans seriously. I received the card of a Blue Shield employee who was the Operations Management Supervisor. She said it was her job to contact doctors who were refusing to accept Covered California health plans and educate them about Blue Shield’s provider obligations. I called the number on the card and was informed that the telephone number was no longer in use. I then sent the information on the doctors to Blue Shield’s Provider Information and Enrollment Services department. I received the following reply.
This is in response to your recent inquiry received 10.27.16, regarding Dr. ABC MD and Dr. XYZ MD being on file with Blue Shield of California as contracted PPO providers with the Covered California networks not accepting members. We do show these doctors as accepting new members but this request has to come from our customer service department so we can contact the doctor’s office for breach in their contract. You would need to call the number on the back of your members card and tell them this so that they can contact our department here in contracting. If you have any further questions please feel free to contact our department phone number or email below.
Once my client had been issued his Blue Shield member ID number I called the Member Services department. I was transferred to the Producers Services department who wanted to transfer me back to Member Services. After much polite back and forth, the Blue Shield customer service representative informed me that Blue Shield could not force doctors to accept health plans from Covered California.
It was obvious to me that something over the last year had changed at Blue Shield. They went from wanting to aggressively educated doctors about not discriminating against Covered California members to shrugging their shoulders over such complaints. They did say that the information was noted and that they did have other complaints about one of the doctors already on file about his refusal to accept Covered California health insurance.
Blue Shield Independent Physician and Provider Manual
Blue Shield Provider Standards
Blue Shield provider Agreements stipulate that Blue Shield providers agree to comply with the following standards. Failure to comply with the standards will be cause for termination of the provider’s Agreement.
Providers agree to deliver quality medical services that are cost-effective and meet prevailing community standards. In the delivery of health care services, providers do not discriminate against any person because of race, color, national origin, religion, sex, sexual orientation, disability, physical handicap, or available benefits. Providers seek to educate and encourage subscribers to follow health practices that improve their lifestyle and well being. Section 2, Page 3, July 2016
I’m not an attorney. But when the provider manual notes doctors are not to discriminate against “available benefits”, I take that to mean that the benefits of the health plan are not to be a cause to reject providing services to a member. In other words, regardless of whether it is a Platinum plan or a high deductible health plan, the doctor cannot discriminate against a Blue Shield member. Of course, nowhere in the manual does it state that doctors can’t discriminate against plans purchased through Covered California.
Covered California members are not second-class citizens
One can only ascertain that in the absence of any language forbidding the discrimination based on Covered California enrollment, Blue Shield has chosen to allow their in-network doctors to refuse health care services to individuals and families of Covered California. Individuals and families who purchase health insurance through Covered California are not second-class citizens. They should not be denied access to health care services based solely on their income level and eligibility for ACA Premium Tax Credits. Doctors who refuse to accept individuals with Covered California health plans are engaging in discriminatory behavior no different from the real estate industry who redline households based on income or skin color.
One Individual and Family Network
As it has been explained to me, Blue Shield, and many of the other carriers, have one Individual and Family Plans (IFP) network of providers. Regardless of whether the plan was purchased directly with the carrier, off-exchange, or through Covered California the IFP network is the same. A search on any of the carrier’s online provider search tools also confirms this. (The provider online search tools can be confusing and complicated.) As for Blue Shield, the main selection is 2016 Individual and Family PPO Plan (including Covered California). There is no differentiation between an off-exchange plan and one purchased through Covered California.
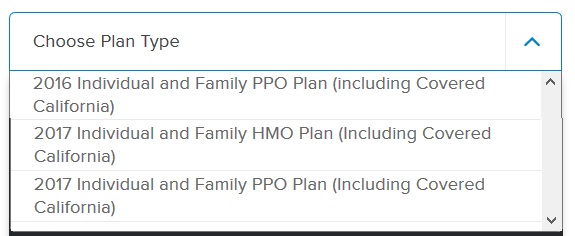
Blue Shield online provider search tool does not differentiate between off-exchange plans or those purchased through Covered California.
Why would a doctor discriminate against Covered California?
Some people have asked if the reimbursements are lower for Covered California health plans. The carriers say this is not the case. They reimburse the provider at the same rate regardless if it is an off-exchange plan or not. Yet, some doctors either refuse to accept Covered California health insurance or stipulate that they only accept Gold and Platinum plans.
So why would a doctor accept an off-exchange plan over a Covered California plan? The rational I have heard most often is to reduce their exposure to unpaid services. Most Covered California individuals and families are receiving a hefty subsidy to reduce their monthly health insurance plan premium. The logic is that if a consumer can afford to pay the full premium amount for an off-exchange plan, they have a higher probability of paying for their office visit and any services rendered by the doctor at the time of the visit.
High Deductible Health Plans Equal High Medical Bills
A patient with a Bronze plan, with a medical deductible of $6,000, may be responsible for the full negotiated rate of any services provided by the doctor. In other words, unless the health plan member had met the high deductible, they would have to pay the full amount for any number of services the doctor may provide during the office visit. If the patient is receiving a subsidy from Covered California, they may not have the cash to pay for those services. This means the doctor may not be able to collect for the services provided.
This leads doctors to only accepting Covered California Gold and Platinum plans that have no deductible. What the doctors may not be aware of is the number of individuals who qualify for Enhanced Silver plans with cost sharing reductions. An individual with a Silver 94 plan, actuarially better than a Platinum 90 plan, have deductible of $75, office visits of $5, and 10% coinsurance. People with an Enhanced Silver plan may be in a better position to meet their health care services payment obligations than those folks paying the full premium amount for a Silver 70 plan.
Send the patient to an out-of-network location
Another trick we have seen doctors using is only accepting Covered California patients at out-of-network locations. The doctor may be listed as in-network for a specific office location. But when a consumer with an individual and family plan makes an appointment, they are directed to another office location. This other office location is under a different medical group that is NOT in-network. The consumer is then billed for out-of-network services and has to fight with the insurance carrier.
Blue Shield, you are better than this
If Blue Shield has really decided to allow their contracted doctors to discriminate against Covered California health plan members, they should openly state it on their website. They should tell the consuming public that they have granted the right to doctors to make a value judgement on the worth of their members based on whether they enrolled directly with Blue Shield or through Covered California. If they are going to allow discrimination to be practiced, they should have to alert consumers to that fact.
[wpfilebase tag=file id=1840 /]


