Covered California consumers who enrolled on or after February 18, 2024, should confirm they paid their initial payment online or contact Kaiser Permanente at 888-236-4490 to make a payment to effectuate their coverage.

Kevin Knauss: Health, History, Travel, Insurance
Posts related to Kaiser Permanente health plans in California for individuals, families, small groups, Covered California.



Unbeknownst to many people, most California health plans cover emergency care anywhere in the United States and treat it as if it were in-network. This means that if you have a Silver 70 plan and are rushed to the emergency room of the nearest hospital while on vacation in upstate New York, your copayment will be $400 just as if the emergency services were performed at your local home office.


This is a review of the responses to the Coronavirus Covid-19 health care issues from the websites of most of the individual and family plan carriers in California. Some websites detail the response and cost of Covid-19 health care issues better than other. They all seem to be covering Covid-19 testing at no cost. The cost of other health care services are subject to the plan benefits.



Kaiser is unique in that because they manage their own pharmacies, we can get a look at the ordering habits of opioids, and by extension, the prescribing of those opioids by Kaiser doctors. With a pharmacy like Costco, that has a higher ordering rate for higher strength doses of hydrocodone, it is hard to pinpoint which doctors or medical groups are prescribing the stronger drugs. It may not even be a doctor in Sacramento County.

If you take a nasty spill on your skate board in San Francisco, and have to have your ankle X-rayed at Kaiser, it will cost $102. But if you break your finger poking your political opponent in the chest, that finger X-ray will cost $111. These costs are lower in Southern California where they have more skate boards and finger poking. An ankle X-ray in Southern California will be $71 and the finger at $78. They don’t mention if there is a discount X-ray cost for both if you poked someone and then fell off your skate board.

By Kevin Knauss

Kaiser Permanente has seen their market share increase with the Affordable Care Act. Their percentage of Covered California enrollments has steadily increased from 24% in 2015 to 33% in 2018.They have also been very stable in their plan offerings on and off exchange. Kaiser rates increased 3% – 7% in Northern California and 6% – 10% in Southern California in 2018. In 2019, the average rate increase will be 9% throughout California.


So why is this significant? Because Kaiser was sending statements to the Covered California household for past due balances greater than one month. They were also sending termination notices even though they had already sent Covered California cancellation of the plan and Covered California terminated the enrollment. But Covered California will not investigate the erroneous terminations. They just tell the agents and consumers they have to deal with the health plan. In this case, the family has sent voluminous amounts of documents to Kaiser showing they made their premium payments.
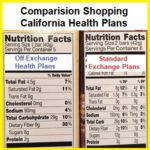


Health insurance companies are smarter than your average house cat. They have reams of data about health care claims and demographics. They can forecast, with reasonable confidence, that altering some of the member cost-sharing benefits may reduce their final exposure to pay member claims. It has also been suggested that consumers who purchase health insurance off-exchange, paying the full premium rate with no subsidy, may be more judicious in how they use health care services. In other word, off-exchange consumer mays tend to file fewer health care expense claims. This results in lower rates to the consumer.


The health plans and Covered California may give lip service to the value of the agent community, but it is not reflected in the compensation we receive. I’m not trying to get rich as an insurance agent. My net revenue listed on my Schedule C for 2016 was $34,000. If the new compensation schedules significantly erode my insurance revenue then I will have to find other income streams. Maybe Covered California will hire me to answer phone calls; I hear they have a great benefits package.

Spam prevention powered by Akismet