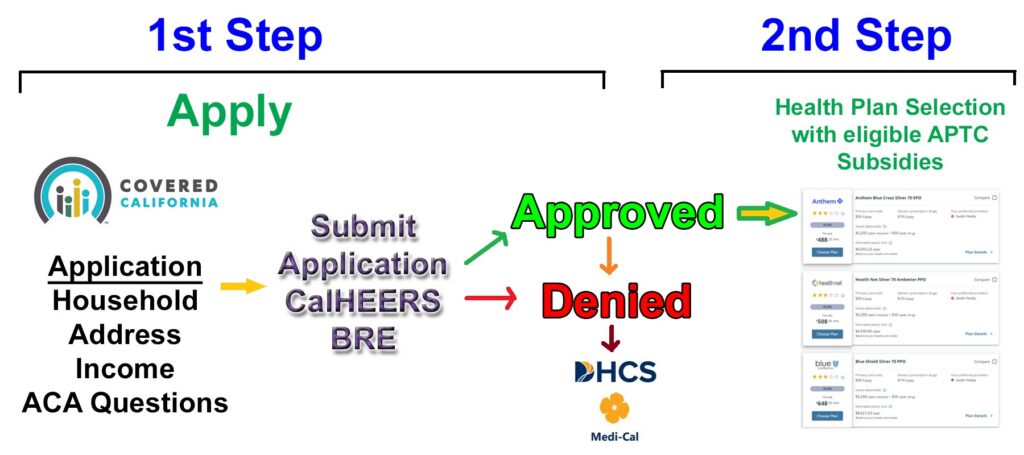
Covered California is 2-step process where you must first apply and be determined eligible for health insurance and the subsidy. The second step is selecting a health plan. There is a mysterious middle section that can present problems for some households with previous Medi-Cal enrollment.
Step 1 is to Apply through Covered California
The first step is to apply through Covered California to determine if you are eligible for health insurance with a Premium Tax Credit subsidy to lower the monthly premium. You will need to answer a series of questions such as dates of birth, address, income, immigration status, and your tax filing status.
Once you completed the online application, you submit it and it is process through the California Healthplan, Eligibility, Enrollment, and Retention System (CalHEERS) program that is the mysterious middle. The answers on the application will determine if you are approved, denied, or are eligible for Medi-Cal
Step 2 is Selecting a Health Plan with the Subsidy
If you are approved, you move to step 2 where you select a health plan with any subsidy applied. The subsidy is paid by Covered California to the health plan you select.
The mysterious middle section is where the application is run through the business rules engine of CalHEERS. The program compares your answers to the necessary eligibility criteria. For example, if you are applying outside of the open enrollment period and you don’t have the correct qualifying life event for a special enrollment period, you are denied. The denial may be a date error on your part or the incorrect selection of the qualifying life event.
If your monthly income is too low, you or your dependent children may be determined eligible for Medi-Cal. The Covered California application is very date sensitive. You need to have the correct dates of income sources in order for them to be properly calculated for the monthly and annual income estimate.
Mysterious Medi-Cal Middle

There can other potential application errors if you are transitioning from Medi-Cal to Covered California. Your county Medi-Cal eligibility worker updates your information directly into the application. However, we have seen where the updated information is correct, but the application has not been run through business rules engine of the process. This can lead to inaccurate eligibility results and Premium Tax Credit subsidies.
As a check to confirm the results are correct, use the Covered California Shop and Compare tool. It is very accurate and will tell you if you and your children are eligible along with the estimated subsidy. If the results are significantly different from what Covered California shows in your account, you need to carefully scrutinize the application from the Review Application tab on your home page.
Finding, Correcting Application Errors
When you scrutinize the application entries, you may discover a simple error or omission that Medi-Cal has made that prevents you from receiving the subsidies. It can be as simple as not having the box “Required to File Taxes” check marked. If your application doesn’t indicate you plan to file taxes, you can enroll in a health plan, but Covered California can’t offer any subsidy.
If the application looks correct, but the results are suspect, you can always submit Report a Change – without making any changes to the application – and resubmitting through the system. The CalHEERS program will run the application like it is new. This will apply the correct information and hopefully return a result similar or exactly like the Covered California Shop and Compare tool.
I have seen where the information all looks correct, but Medi-Cal never resubmitted the application. Medi-Cal changes their database and that of Covered California. However, if those changes are not properly processed through CalHEERS, your results may not be correct.
It is important to ensure that Covered California is calculating the correct subsidy for your health plan. If Covered California, based on incorrect information, forwards too much monthly subsidy, then you will have to repay a large excess amount of the Premium Tax Credit when you file your federal tax return for the year.