Consumers are growing frustrated as they find their current doctors aren’t included in new Covered California individual and family plan (IFP) health insurance networks. There is also widespread uncertainty about the rules of in-network providers with the new Exclusive Provider Organizations (EPOs) and California’s new 19 pricing regions. When California consumers are craving information the doctors have been silent and the insurance companies along with Covered California are providing scant information.
Which doctors are really in-network?
The first challenge for consumers in determining if their current physicians were “in-network” with the new plans was consulting the online search tools. All of those search functions were unreliable until November. (I’m still not certain that Covered California’s search tool is accurate). When people and agents did get serious about finding which doctors were in the PPO, EPO, and HMO networks, consumers found out that the availability of in-network doctors had drastically shrunk in some areas.
Doctor offices clueless as to networks
A client recently found out that the doctor he has seen for years will no longer be included in his PPO network. Dr. X in Fair Oaks, CA, is in neither the Anthem Blue Cross or Blue Shield of California network for IFP PPOs. Neither the client’s current health plan nor Dr. X notified him of this change. When I called the doctor office to confirm he was not in-network I was referred to the billing person, who referred me to the person who handles the contracts, who in turned referred me to Hills Physicians Groups who Dr. X is associated with. No one gave me an answer.
Money equals access
The client finally called the office and was told that Dr. X was not participating in any of the new Obamacare ACA individual health plans. As one would suspect; that information was wrong. Dr. X is listed, and can be chosen, as a primary care physician with the HMO of Western Health Advantage (WHA). Unfortunately, the Silver plan from WHA which includes Dr. X is $130 more per month than either the Anthem Blue Cross or Blue Shield and as my client travels extensively, an HMO is not the best option.
Who is to blame insurers or doctors?
The response and lack of knowledge about health plans from Dr. X’s office is similar to other providers I have called: clueless and confused. Physicians and health plans owe my client and thousands of other current and soon to be former patients an answer. Why are these doctors no longer in-network? Are the insurance companies arbitrarily dropping doctors because they want a reimbursement for services that is too high? Are the doctors abandoning insurance plans because they don’t pay enough?
CMA advocates for transparent networks
The California Medical Association that says they represent over 38,000 physicians has been relatively silent on the new health plan networks. From their website they note, “The association was founded in 1856 by a small group of physicians who knew it was their duty to fight for their patients and for their profession.” I guess they lost the drive to fight for their patients whose physician is no longer in-network. One of CMA’s top issues is “Advocating for adequate, accurate and transparent provider networks;”
No help for provider networks
While CMA seems to be ignoring the provider network complaints, they are are quick to accept a $1.5 million grant from Covered California to educate their members about the new exchange (Foundation’s Covered California educational program moves into high gear). I suppose they’ll ignore those areas where few of their members participate in PPO plans. CMA is also strong in advocating against cuts to Medicare reimbursement for their physicians (2014 Medicare fee schedule confirms 24 percent cut). They also go the extra-mile to help their members get reimbursed from insurance companies (We help you get paid) and other resources to help insure the highest reimbursements rates from health plans called Silent PPO Action Guide.
Single payer socialized Medicare has more providers
One of the largest nationwide PPO networks is administered by the single payer plan called Medicare. Anecdotally, it seemed like there more physicians available to the socialized medicine recipients in Medicare than the new private enterprise health plan networks. I searched available providers by zip code in various cities to see how many were available. The results are not perfect, but I tried to make the searches as consistent as possible between Original Medicare and new 2014 IFP PPO plans offered by Blue Shield, Anthem Blue Cross and Health Net.
The search for PPO network doctors
Each of the respective doctor online search engines is slightly different. The two variables that were apt to cause the most difference in results were the types of physicians being sought and the distance or radius from the zip code entered. By default, the Medicare.gov search may include a higher number of physicians because it included Geriatric medicine where the other searches did not. I also adjusted the radius of the search to be as close to the pre-determined Medicare distance as possible.
Search terms
- Medicare: Family Practice, General Practice, Geriatric Medicine, Internal Medicine, and Primary Care Physicians is predefined on the Medicare website.
- Anthem Blue Cross: Family, General, Internal, OBGYN
- Blue Shield: Family, General, Internal, OBGYN
- Health Net: Family, General, Internal, OBGYN
PPO Doctors by City by Health Plan
| Medicare | Blue Shield | Blue Cross | Health Net | |
| Redding | 142 | 115 | 117 | 0 |
| Eureka | 59 | 48 | 44 | 0 |
| Carmichael | 204 | 58 | 92 | 0 |
| Oakland | 225 | 102 | 123 | 0 |
| Mill Valley | 89 | 32 | 19 | 35 |
| San Francisco | 1296 | 169 | 2 | 268 |
| Stockton | 105 | 27 | 78 | 72 |
| Chowchilla | 122 | 74 | 216 | 0 |
| Bakersfield | 198 | 46 | 131 | 93 |
| Santa Barbara | 144 | 5 | 113 | 0 |
| Van Nuys | 499 | 32 | 0 | 152 |
| Beverly Hills | 1274 | 27 | 0 | 309 |
| Anaheim | 285 | 119 | 0 | 227 |
| San Diego | 1009 | 68 | 0 | 158 |
| Totals | 5651 | 922 | 935 | 1314 |
0 physicians results from no IFP PPO plan being offered by the insurance company in the region. Full spreadsheet of data at end of post.
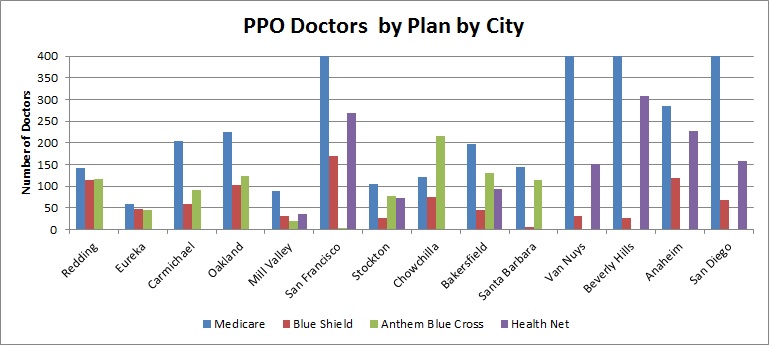
Single payer Medicare has more doctors than private health insurance plans.
Network questions
California consumers and agent are getting conflicting answers regarding the new networks as well. The big question is whether a PPO plan member can see health plan network physician in another plan region and have the visit fall under their in-network copayment and coinsurance structure? Are Exclusive Provider Organization (EPO) physicians considered in-network for PPO members? This is still gray area it may not be resolved until all the carriers release their Evidence of Coverage (EOC) documents for each plan.
EPO, PPO, HMO, Tiered network consumer confusion
Blue Shield has released their EOCs which show that PPO members can still use Blue Card physicians in other state as in-network. Anthem Blue Cross and Blue Shield have indicated verbally that PPO members can see any network physician listed on their provider search engine as in-network. But will that apply to facilities like hospitals and out-patient facilities? Will the “any network provider” apply to $0 copay preventive services? We know that neither Anthem Blue Cross nor Blue Shield will honor the $0 copay preventive office visit or tests when received from an out-of-network provider. See EPO, PPO, HMO networks, which is best?
Insurers, doctors put profits before people?
The Center for Medicare and Medicaid Services mandates that Medicare Advantage plans must notify members in their Annual Notice of Changes if physicians and facilities are no longer in-network for plan members. The same courtesy should be extended to members of IFPs in California. The current system of providers included or excluded from IFPs, small or large group plans, Medicare, PPOs, EPOs, and HMOs has become mind numbingly complicated for consumers. The whole purpose of all the networks is to put profits before people for the insurance companies, doctors and hospitals.
Will California get real answers from doctors or insurers?
The madness needs to end. Californians need the transparency of networks that Covered California promised. Physician groups, doctors and the CMA need to step up to the plate and explain why they are not participating in certain networks and leaving their current patients high and dry.
[gview file=”https://insuremekevin.com/wp-content/uploads/2013/12/health_plan_doctor_numbers.xlsx” save=”1″]


