We are in an era of heightened online precautions focused on keeping personally identifying information private. Yet, with no permission from the individual or family members, Medi-Cal can access a person’s Covered California account and make changes, that at times, lead to errors in the consumer’s health insurance. Has anyone ever given Medi-Cal permission to access their Covered California account?

Recently, a couple retiring and losing employer sponsored health insurance submitted a Covered California application for health insurance. There was a small date error in the reporting of the income. This date error led to the couple being determined eligible for Medi-Cal and not a private plan through Covered California with the health insurance subsidies. The couple delegated me as their Covered California agent and I was able to access their application and correct the income date issue.
Upon resubmitting the application to Covered California, the couple was then offered the opportunity to enroll in a health plan with a subsidy. They made their selection and paid the first month’s premium for the health plan through their Covered California account. They were enjoying retirement when they received confusing letters from Medi-Cal and Covered California.
No one granted permission to Medi-Cal to access the Covered California account
Santa Barbara County sent a letter saying the couple did not qualify for Medi-Cal. They then received a letter from Covered California stating that they no longer qualified for any subsidy. When I accessed the couple’s Covered California account, all of their income information had been erased. When I looked at the transaction history on the Covered California account, Santa Barbara County Medi-Cal office had accessed the account and submitted changes.
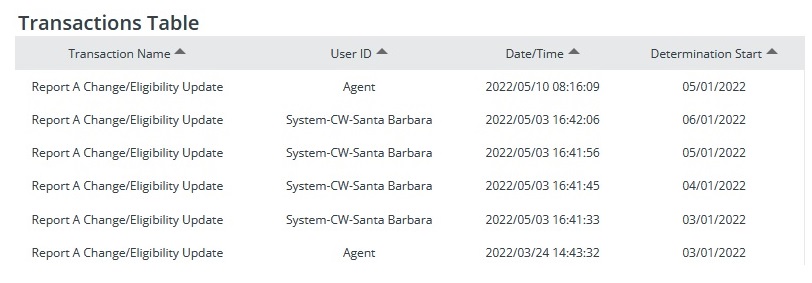
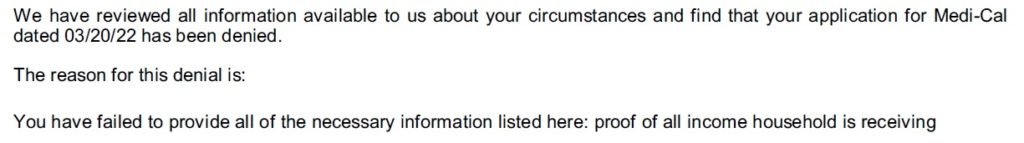
Whatever Santa Barbara County did in reviewing the couple’s Covered California application, they managed to wipe out the couple’s 2022 estimated income. Technically, if an application has no income, the household is determined eligible for Medi-Cal. The Medi-Cal eligibility did not happen. When Santa Barbara submitted the application to update their review and changes, the Covered California CalHEERS application program determined the couple, in addition to not being Medi-Cal eligible, were not eligible for any subsidies.

Fortunately, I was able to rebuild the couple’s income section and when I resubmitted the application, the subsidies returned, lowering their health insurance monthly bill by $1,600, the original subsidy amount.
No Consumer Alert About Medi-Cal Access
When a consumer delegates me as their agent, they must read and check mark several boxes indicating that they understand that I, as a certified insurance agent, will be able to access their Covered California account and make necessary changes authorized by them. Before I submit an application, I must read several paragraphs to the consumer that they must report changes within 30 days, intentional misrepresentations of application information may result in penalties or jail time, that consumers must file a tax return, and Covered California does not discriminate on the basis of race, gender, ethnicity, etc.
No where in the application process is there an alert or disclaimer that a county Medi-Cal office can access the consumer’s Covered California account and make changes without the consumer’s permission or authorization. I have never seen any text that informs a consumer that by enrolling through Covered California the primary tax payer, primary applicant, or other household members grant permission to their county Medi-Cal office to access, review, or change any data the consumer or delegated agent has entered.
There are rules regarding enrollment in a private health plan through Covered California with the subsidies. If the household income is too low, or there is no income, the individual is determined eligible for Medi-Cal and Covered California forwards the information to the respective county Medi-Cal office. I help people become eligible for Medi-Cal all the time by processing a Covered California application that makes the Medi-Cal eligibility determination. The county Medi-Cal office makes the final eligibility and enrollment determination.
If the household has mixed eligibility, adults eligible for Covered California subsidies and children eligible for Medi-Cal, all changes to the Covered California account (income, address, new family members, etc.) must go through the local county Medi-Cal office. This all makes perfect sense and if the consumer does not want Medi-Cal, they can decline the no cost health insurance.
All the rules and transferring of information is meant to structure a system where people do not fall through the cracks of our health insurance sidewalk. However, has the zeal for the mission to get everyone covered with health insurance led the Department of Health Care Services, the parent agency of Medi-Cal, to sacrifice privacy concerns of Covered California consumers?
Unanswered Medi-Cal Access Questions
It was disconcerting to the couple who contacted me that Santa Barbara County Medi-Cal had accessed their Covered California account without their permission. Who was the person who accessed their account? Why did they access the account if they were already properly enrolled in a health plan and paid the first month’s premium? How could they be determined ineligible for Medi-Cal by the county, have their income section erased, and then lose their monthly health insurance subsidies?
In cases like these, I have stopped trying to get answers. No one at Covered California or the Department of Health Care Services will talk to me. Sometimes, ironically, they cite privacy concerns. While I can make changes to a client’s Covered California account, there is a separate authorization process for me to be delegated as an authorized representative of the individual to talk to Medi-Cal on my client’s behalf. Of course, the special Medi-Cal authorized representative form is to protect an individual’s privacy and personally identifiable information.
The bureaucratic privacy steamroller continues with the implementation Senate Bill 260. SB 260 mandates that health plans must share contact information with Covered California when a member’s health plan terminates. The health plans are required to forward the names of adults covered on the terminated health plan, contact information such as mailing address, phone, and email address, and the date of the coverage ended.
Health plan members can opt out of the notification. The health plan member’s delegated agent cannot opt out of the program on the member’s behalf. I opt out of receiving spam emails all the time, but I continue to receive the email correspondence regardless.
In general, Covered California and Medi-Cal are doing a good job of implementing their programs. The security protocols are pretty good at Covered California. To create a Covered California account, you have to answer a variety of security questions and create a secure password. As an agent, Covered California makes me change my password every 3 months and I have to review best practices for securing a client’s personal and health information. Covered California is very security and privacy conscience.
Then, Covered California lets unknown and unauthorized Medi-Cal workers access Covered California accounts, make changes, and throw the lives of Californians into chaos. My gut says that somewhere, buried in some obscure legislative act authorizing the California Health Benefits Exchange (aka Covered California), Medi-Cal has primacy over Covered California and can access any account anytime they deem fit.
If such authorization exists, Covered California should alert consumers that their local county Medi-Cal office can access their accounts without their permission or knowledge. In the eyes of most Covered California consumers, Medi-Cal is a third party. Their personal information should not be shared with a third party unless they are able to authorize the sharing of such information. The option to authorize the sharing of personal information with third parties is standard procedure in many consumer agreements.
It is almost funny that social media apps have more third-party sharing notices and authorizations than Covered California does. The end result is that a small number of Medi-Cal goofs and unauthorized changes creates an atmosphere of distrust on the part of consumers toward government programs. For all the good that Covered California and Medi-Cal have done getting affordable health care to people, they undermine their reputation and mission by failing to provide basic consumer information regarding personal account access.


