
Getting and Keeping Health Coverage, A Guide For Advocates to Medi-Cal
The Western Center On Law & Poverty has put together a comprehensive guide to the Medicaid program in California known as Medi-Cal. Published in March 2016, there are bound to be changes to many of Medi-Cal’s programs, conditions, and eligibility in 2017. Titled Getting and Keeping Health Coverage for Low-Income Californians: A Guide for Advocates is 375 pages long and covers many topics from eligibility, citizenship, enrollment, re-determination, and the variety of programs Medi-Cal offers such as Children’s Health Insurance Program, Medi-Cal Access Program (MCAP) for pregnant women.
Medi-Cal Highlights From An Advocates Guide
I’ve noted some of the highlights that apply to MAGI Medi-Cal and Covered California as outlined in the guide. There is an exception for almost every guideline or rule presented. While the guide provides a fair amount of specific details on the variety of programs administered by the Department of Health Care Services and county social services Medi-Cal departments, there can be specific conditions for eligibility not mentioned in the guide.
[wpfilebase tag=file id=1670 /]
Introduction: Eligibility At-A-Glance
Household
The guide address both the expanded Medi-Cal based on a household Modified Adjusted Gross Income (MAGI) and Non-MAGI programs such as health insurance for the aged, blind, disabled, foster children, refugee, or those with specific medical conditions. For Covered California, which screens for MAGI Medi-Cal eligibility, the household includes the tax payer and all members claimed on their federal income tax return.
Assets or Resources
The MAGI conditions for eligibility of the expanded Medi-Cal program do not consider assets or resources other than income. Applicants for MAGI Medi-Cal, Medi-Cal Access Program for pregnant women are not asked about bank accounts, homes, cars, or other property. (However, some applicants have received eligibility notices from county social services departments requesting asset information, which is confusing.)
Chapter 1: Overarching Eligibility Issues for Medi-Cal
Immigration
Lawfully present individuals are eligible for full-scope Medi-Cal benefits. Qualified immigrants are those individuals who are Permanently Residing Under the Color of Law (PRUCOL). The guide lists several categories of qualified immigration status for Medi-Cal. There is generally a five year waiting period for immigrants to obtain Medicaid. California has decided to offer full-scope Medi-Cal to lawfully residing immigrant children and pregnant women without a waiting period. California uses state funds to offer Medi-Cal to non-pregnant adults and other lawfully present immigrants who may not be eligible for benefits. The guide discusses PRUCOL and Restricted Scope Medi-Cal benefits.
Chapter 2: MAGI Medi-Cal Programs
Household
Unlike eligibility for Covered California tax credits, Medi-Cal eligible individuals and households may be required to file taxes. Consequently, there are tax-filer and non-tax-filer rules. Individuals in the same family may be part of different households as well. For example, for Medi-Cal Access Program a single pregnant woman with no other children is counted as a household of two or more.
Income
Income for MAGI Medi-Cal closely aligns with Covered California. Income consists of taxable income from a job or self-employment, Social Security benefits, tax-exempt interest, and foreign earned income. There are some difference between MAGI Medi-Cal and Covered California countable income sources.
- One-time lump sum income is only counted in the month received for Medi-Cal. Technically, the individual or household would lose Medi-Cal for the month the one-time lump sum is received. MCAP is excluded from the loss of coverage due to the lump sum distribution.
- Scholarships or fellowship grants for education expenses are excluded.
- American Indians and Alaska Natives can exclude several tribal-related sources of income.
- Counties, who administer Medi-Cal eligibility, can base Medi-Cal enrollment on monthly income rather than annual.
Expanded MAGI Medi-Cal programs are available to
- Adults whose income is below 138% of the federal poverty level
- Parent and Caretaker Relatives with income below 109% of the federal poverty level
- Pregnant women with income below 213% of the federal poverty level
- Pregnant women with income between 213% and 322% of the federal poverty level, Medi-Cal Access Program.
- Children Ages 1 to 19 years old: with household income up to 160% of the federal poverty level are eligible for no-cost Medi-Cal. Income between 160% and 266% of the federal poverty level are eligible for Medi-Cal with monthly premiums. Targeted Low-Income Children’s Program.
Individuals must not be eligible for Medicare Part A or B.
Chapter 3: Non-MAGI Medi-Cal
This chapter deals with the variety of programs for individuals based on disability, foster youth, and Medicare.
Chapter 4: Covered California
This chapter deals with enrolling in health insurance through Covered California and the eligibility for the Premium Tax Credits. As the guide mentions the Covered California online application CalHEERS (California Healthcare Eligibility Enrollment & Retention System) is the Business Rules Engine (BRE) for screening applicants for eligibility for either a private health plan with tax credits or Medi-Cal eligibility. Even though CalHEERS was designed to be the default enrollment and eligibility system, Medi-Cal also has a couple of other software systems to enroll and track Medi-Cal members.
Medi-Cal Enrollment
If an individual is deemed eligible for Medi-Cal, the insurance is retroactive to the first day of the month in which they applied. Medi-Cal can actually be retroactive up to three months prior to enrollment if they were eligible. In some situations, Medi-Cal can be retroactive up to 12 months prior to the application date. Unlike Covered California private health plans where households can only enroll during the fall Open Enrollment Period or with a qualifying event for Special Enrollment, Medi-Cal is open year round. The Medi-Cal Access Program coverage starts 10 calendar days after the date of the application is approved.
Most MAGI Medi-Cal members must enroll in managed HMO health plan offered through their county. They will receive a packet of information about choosing a Medi-Cal health plan if more than one plan is offered in their county. If a member does not select a plan, the county will enroll the person in one. For women eligible for MCAP, if two plan options are offered, they must select a plan or they will not be enrolled.
Chapter 6: Staying On Coverage
This chapter deals with keeping Medi-Cal coverage while reporting changes for the household to Medi-Cal.
The guide states that consumers can manage their Medi-Cal coverage and report changes through their Covered California account. This really isn’t the case. If an individual is on Medi-Cal, or a household has a family member enrolled in Medi-Cal, virtually all changes need to be reported to the county social services department. This is especially true with changes to income. An increase to the household income that may lift some or all household members out of Medi-Cal must be reported to the county for verification.
Re-determination
In the absence of any reported changes from the household, Medi-Cal eligibility is re-determined every 12 months. Medi-Cal beneficiaries must report all household changes within 10 days to Medi-Cal. This includes changes to income, additional household members, members who have left, address change, immigration status, incarceration, or access to other health coverage. Medi-Cal members receive a pre-populated MAGI Medi-Cal Annual Renewal form MC 216. Medi-Cal beneficiaries have 60 days to confirm or correct the information on the MC 216. If the Medi-Cal beneficiary does not respond, they receive a ten-day Notice of Action regarding termination.
Medi-Cal will review all available data sources, in addition to changes reported by the beneficiary, to make an eligibility determination. This might include information from CalWORKs and federal data services hub. If the household is determined to be no longer eligible for Medi-Cal, they will receive a ten-day Notice of Action alerting them to the termination of Medi-Cal benefits. County Medi-Cal offices will coordinate termination with Covered California so that the household can enroll in a private plan with or without financial assistance and have no gap in coverage. This usually means that Medi-Cal is terminated at the end of the month. Loss of health coverage is a qualifying event for a Special Enrollment Period into Covered California or directly with a health insurance plan off-exchange.
Covered California is supposed to review member accounts twice a year to determine if there may be any changes that make the household eligible for Medi-Cal or ineligible for the tax credits. The review screens for household members who may have died or become eligible for Medicare. Covered California must give members 30 days to respond to any data changes that they find.
There generally is no redetermination for MCAP coverage. Women should notify Medi-Cal if their pregnancy condition changes, such as birth, or a drop of income.
Medi-Cal Portability
Medi-Cal is portable. If a beneficiary moves, they do not have to re-apply. Their Medi-Cal benefits will be transferred to the new county they move to. Upon notification of an address change to a new county, the Sending County initiates Inter-County Transfer. The Receiving County will receive updated beneficiary information that is updated in the Medi-Cal Eligibility Data System (MEDS).
Under state law (SB 87), Medi-Cal must screen all beneficiaries for eligibility for other state and Medi-Cal programs. This means households may receive information or enrollment into other programs such as CalFresh. The point of the evaluation is to ensure that a termination of Medi-Cal doesn’t leave a person without coverage if indeed they may be eligible for Non-MAGI Medi-Cal or other programs like MCAP.
Mega Mandatory Groups
Some Medi-Cal beneficiaries fall into the Mega Mandatory group and may not have to undergo the annual re-determination for eligibility. In other words, some individuals that qualify under rules for disability or foster youth will continue to be eligible for Medi-Cal without the re-determination process of either MAGI or Non-MAGI Medi-Cal. Mega Mandatory beneficiaries are generally not included in the tax household when determining eligibility for other household members for Medi-Cal.
Mixed Households
Families can have some members with Covered California health plan tax credit assistance and other household members, usually children, in Medi-Cal. The Medi-Cal re-determination may be different from the Open Enrollment Period for Covered California health insurance. All changes for the household must also be submitted to the county Medi-Cal office even if some members are in a private health plan through Covered California.
Medi-Cal Denial Appeal
Medi-Cal beneficiaries or individuals who think they should have Medi-Cal benefits can appeal a decision of ineligibility. Medi-Cal applicants can request a Fair Hearing and can be represented by an authorized representative. Beneficiaries terminated from Med-Cal for lack of information to re-determine their eligibility have 90 days to get back into Medi-Cal. It will be retroactive if approved. Some beneficiaries may be able to keep their Medi-Cal benefits if they request a Fair Hearing within ten days of the Notice of Action of termination. The appeals process can be lengthy and there are several types of appeals and deadlines for information as noted in the guide
Covered California to Medi-Cal
If Covered California determines that a consumer is no longer eligible for a health plan with premium tax credits they must provide the household a 14 day notice before the effective termination date. If the consumer appeals the decision they have the right to remain in their health plan while the appeals process is completed. If they are ultimately deemed ineligible for Covered California, they may owe back premium tax credits.
Chapter 7: Counties’ Legal Obligation to Provide Care to Remaining Uninsured
This chapter reviews other programs for cost-sharing, medically indigent, and scope of services for uninsured individuals.
Chapter 8: Options for Hospital Bills
The Hospital Fair Pricing Act requires hospitals and emergency room physicians to offer discount payment plans to individuals who do not qualify for Medi-Cal or are uninsured. Uninsured patients who are below 350% of the federal poverty level are eligible for a hospital’s charity care program. Emergency room physicians can charge no more than 50% of the median billed charges.
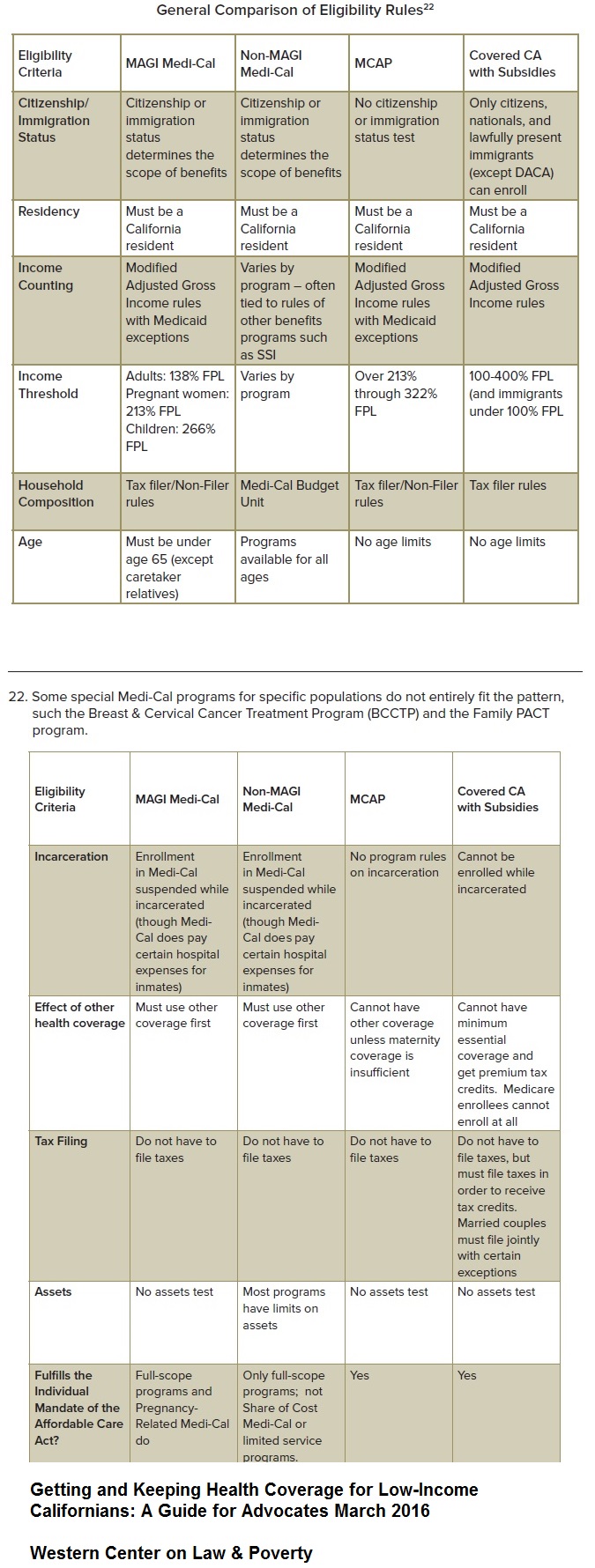
Table of Medi-Cal eligibility under the Affordable Care Act expanded Medi-Cal, MCAP, and Covered California.


