
People don’t trust the concept of Medicare For All because of the bureaucrats who operate Medicaid programs. On a daily basis, with no warning and no authorization, Medi-Cal eligibility workers change the accounts of Covered California members enrolled in private health plans. These unauthorized changes throw individuals and families off of their private health plans and into Medi-Cal, regardless of the treatment the person may be receiving under their current health insurance.
Medicaid is known as Medi-Cal in California. Covered California is the Affordable Care Act market place exchange where individuals and families can be determined eligible for the premium tax credit subsidies to lower their monthly health insurance premiums. Covered California, because they are under the Department of Managed Health Care, also determines if individuals, families, or children are Medi-Cal eligible.
Based on household size and income, if a person is eligible for expanded MAGI Medi-Cal under the Affordable Care Act, Covered California sends that information over to the individual’s local county Medi-Cal agency for enrollment. California counties handle the final eligibility determination and enrollment into Medi-Cal HMO managed care plans.
Medi-Cal Can Meddle In Covered California Accounts
What most people don’t realize is that Medi-Cal has access to all of the information in an individual’s or family’s account. In addition, county level Medi-Cal eligibility case workers can make any changes they want to the information in the account. Once Medi-Cal has made a determination that an individual is Medi-Cal eligible, nothing the person changes in their Covered California account makes any difference.
If a person’s private health insurance plan is terminated because Medi-Cal determines the person is no longer eligible for the premium tax credit subsidy, the person must fight with Medi-Cal to restore their health insurance. This sort of unauthorized government intrusion has led to deep distrust of any Medicare For All health insurance concept.
As a Certified Insurance Agent for Covered California I deal with this sort of unauthorized Medi-Cal meddling all the time. The most recent case involved a client whose Kaiser health plan was terminated after Sacramento County Medi-Cal eligibility workers went into the client’s Covered California account and changed her information. Specifically, they put the deceased spouse back into the household! They also lowered the income, which we had updated in 2019 for the 2020 enrollment plan year.
The client’s income had gone up. We were not fudging the income just to keep her out of Medi-Cal income eligibility territory. The client even had to repay some of the Advance Premium Tax Credits she received in 2019 back to the IRS because the final Modified Adjusted Gross Income was higher than we originally estimated.
Medi-Cal Terminates Covered California Health Insurance
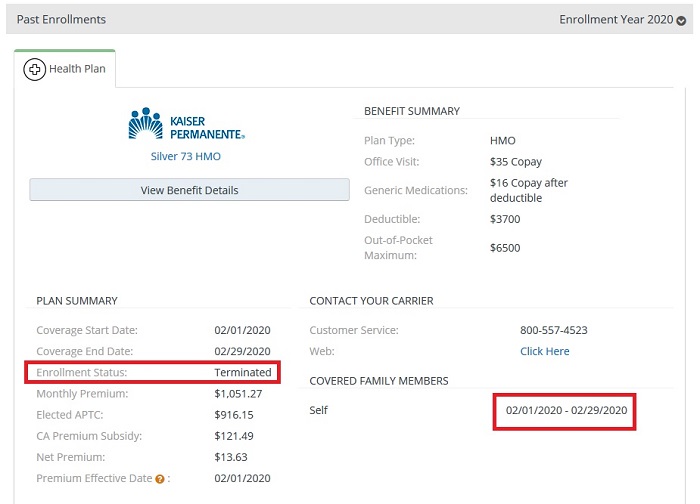
The only notification the client received that Medi-Cal had meddled with her account was when she received a notice from Kaiser informing the client that her coverage had been terminated. Medi-Cal sent no notice that they had made the changes. Covered California sent no notice the changes had been made or that her plan was being terminated.
There is nothing in the Covered California enrollment agreement that alerts consumers that Medi-Cal has broad and sweeping authority to make changes to a member’s account without prior notification or authorization.
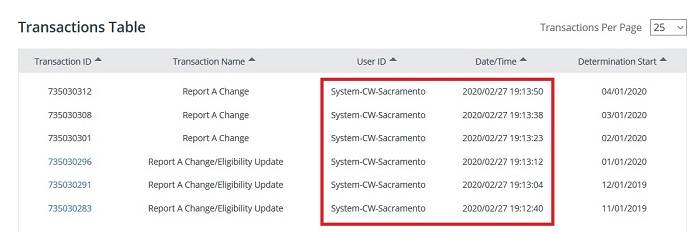
But it is clear from the transaction log from Covered California that Sacrament County Medi-Cal (User ID = System-CW-Sacramento) was in the account at the end of February.
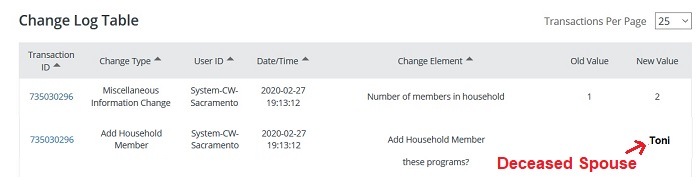
The Change Log Table shows that Sacramento County Medi-Cal returned the client’s household size to 2 and added the deceased spouse back into the household.
Sacramento County Medi-Cal told my client that all the changes were just an automated system. Frankly, I don’t believe it.
The client did call Sacramento County Medi-Cal and they reverted their changes. This allowed us to re-enroll the client into a health plan. But because we enrolled her on March 2nd, the health plan will not start until April 1st. Normally when Medi-Cal terminates a private health plan because they have determined the individual or family is eligible for Medi-Cal, the members of the household will have Medi-Cal at least for that time.
Left With No Health Insurance
Unfortunately, Sacramento County did not even do that. They terminated my client’s Covered California account and left her uninsured. They did not enroll her into a Medi-Cal plan and they have no way of forcing Covered California to easily reinstate the client’s March coverage – which she has already paid for – with Kaiser. The coverage issue has now been escalated at Covered California. It’s a mess.
This is the type of bureaucratic nightmare that makes most reasonable people so opposed to any expansion of a government run health care system. I will say that Medicare, after many years of problems, runs very smoothly for most Medicare eligible individuals. The dread most people have is Medicare’s ability to scale their eligibility and enrollment process to cover all eligible U.S. residents under 65 years of age.
Covered California is running pretty smoothly, for the most part, five years after its launch and numerous growing pains. The chronic problems of Covered California usually revolve around Medi-Cal. The county Medi-Cal eligibility case worker supersedes everyone at Covered California. And what really irks people is that Medi-Cal doesn’t have to seek authorization to touch a Covered California account and they don’t have to notify individuals or families that they will be making changes that terminate their private health insurance coverage.
If Medicare For All smells anything like the unauthorized meddling by a nameless government bureaucrat that is allowed to make changes without consulting the consumer, it will be thumbs down for Medicare For All.


