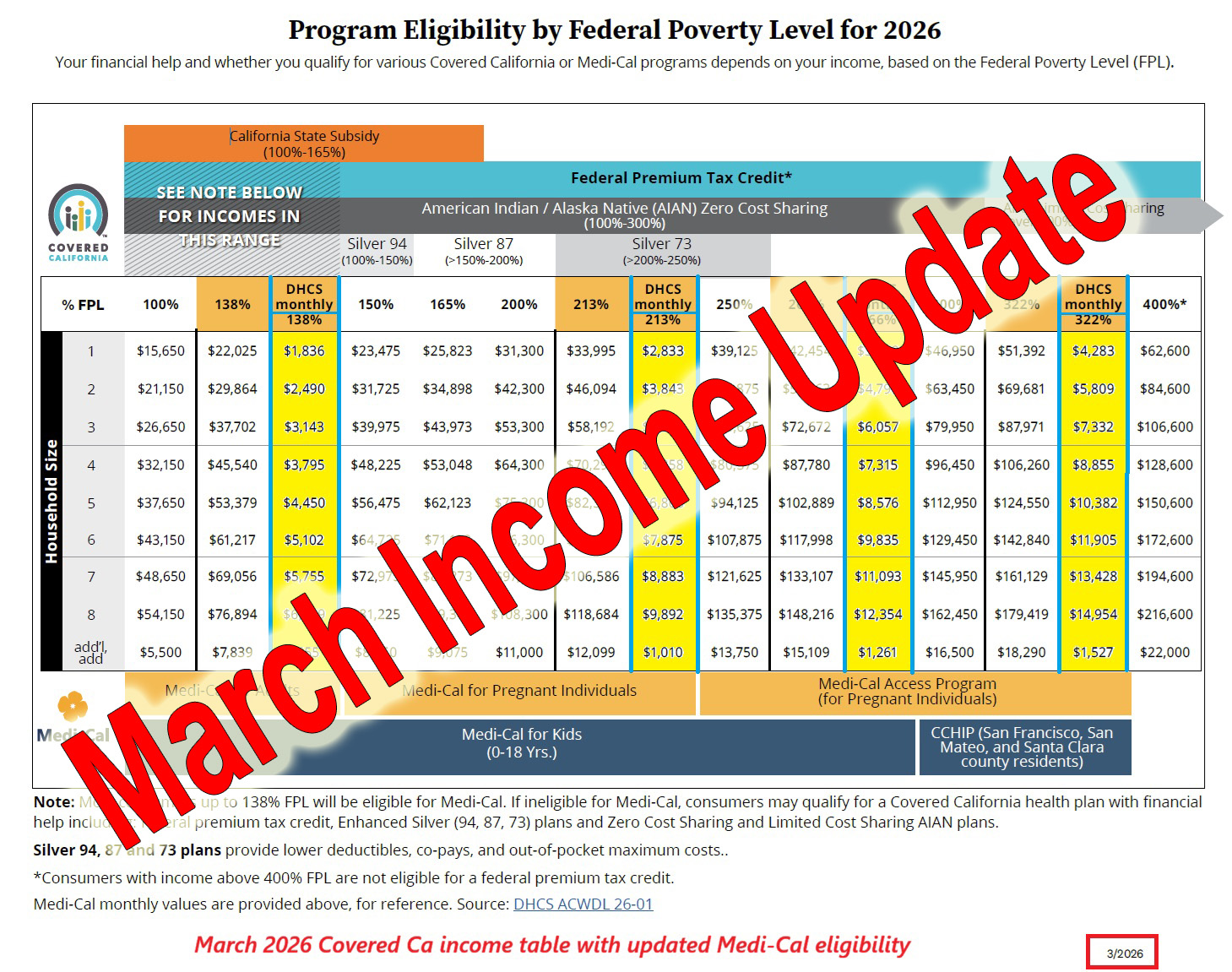
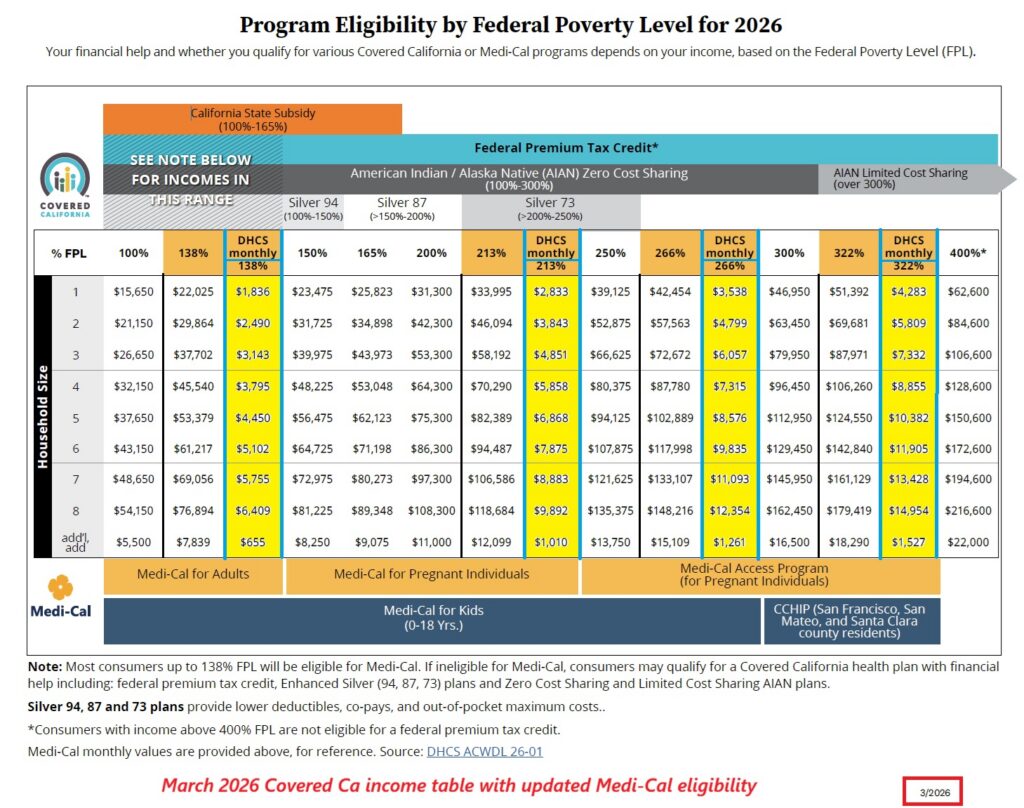
Covered California has revised their income table to reflect the higher federal poverty levels. The higher dollar amount numbers are effective March 2026. The revision only applies to Medi-Cal programs.
When reviewing any income table update, make sure the date in the lower right-hand corner is 3/2026. That is the revised table from the 10/2025 open enrollment income chart. The yellow columns are the monthly amount necessary for Medi-Cal. Your monthly income on the Covered California application needs to be greater than the Medi-Cal monthly amount in order to be eligible for a private health plan with a subsidy.
Only the columns in orange/yellow increased based on the 2026 higher federal poverty level. All other columns that apply to enhanced Silver plans remain the same as the open enrollment income table.
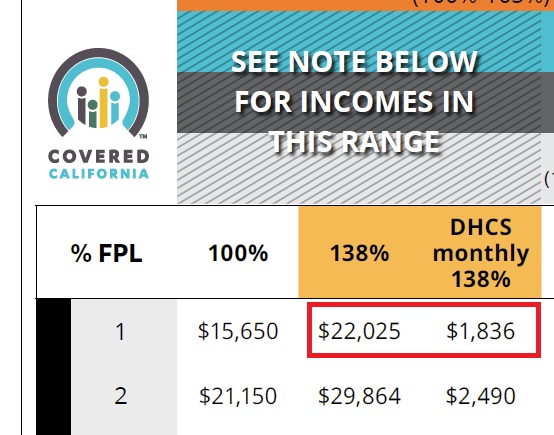
Effective March 2026, single adults applying to Covered California will need to have a monthly income more than $1,836 to be eligible for a private health plan with the subsidy. Monthly incomes lower will be Medi-Cal eligible.
For two adults, the monthly income must be greater than $2,490 per month for Covered California.
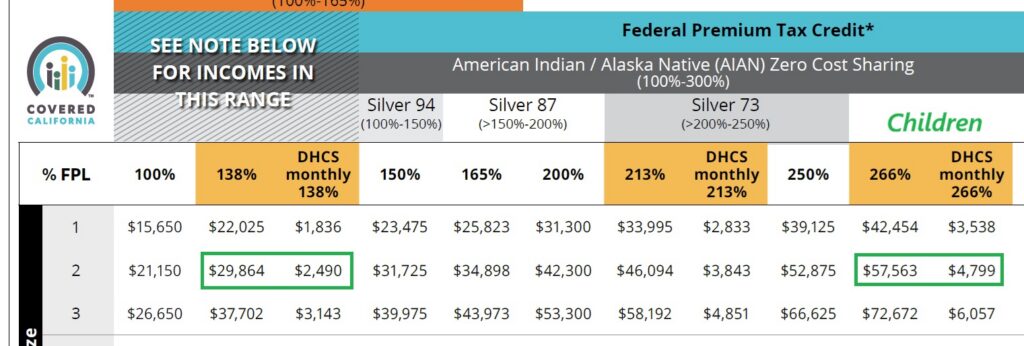
For a household of two, one adult and one child, the monthly income must be greater than $4,799 for the child to receive a subsidy and not be Medi-Cal eligible.
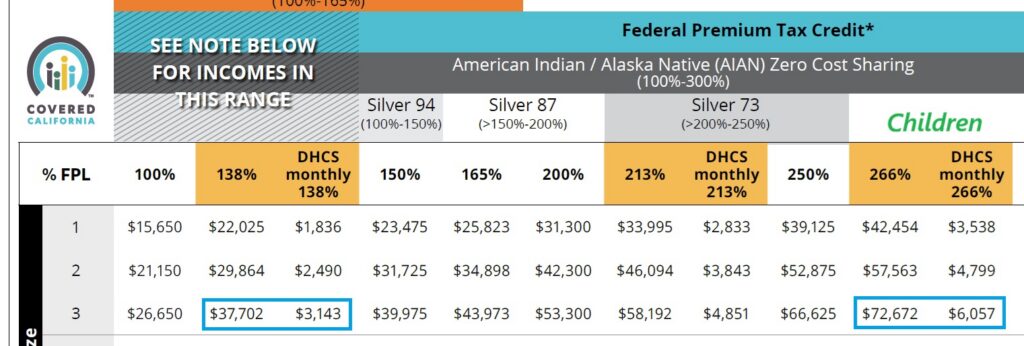
In a household of three, the monthly income must be greater than $6,057 for children to be eligible for Covered California.
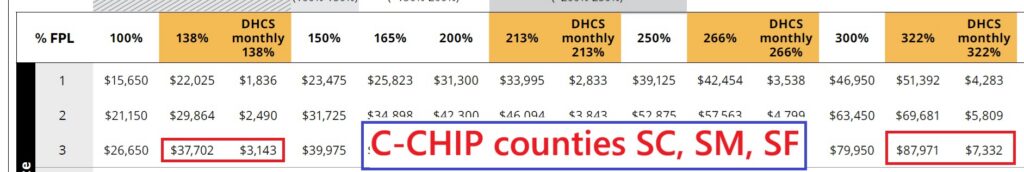
The monthly income for children to be eligible for Covered California is higher in C-CHIP counties of Santa Clara, San Mateo, and San Francisco. The monthly income must be greater than $7,332 in the household of three scenario.
The higher Medi-Cal eligible monthly income amounts will be applied to new applicants or current Covered California consumers if they report a change beginning in March.
YouTube video on revised March Covered California income table.