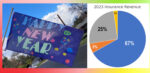
Commissions from the various health, dental, and vision plans I represent totaled approximately $87,000 in 2023. Insurance commissions equaled 92 percent of my total revenue. Google and YouTube advertising revenue accounted for 2 percent of income and a few crumbs from book sales.