
For several years after the launch of Covered California, if a woman indicated she was pregnant in her Covered California account, she was automatically deemed Medi-Cal eligible regardless of her income or desire for Medi-Cal. Covered California has updated their software to allow women to indicate they are pregnant and then select whether they want to be determined eligible for Medi-Cal.
There is no rule that mandates that a woman who is enrolled in a health plan through Covered California must report that she is pregnant. Becoming pregnant is not a Qualifying Life Event (QLE) for a Special Enrollment Period (SEP) to change health plans or enroll in a health plan outside of Open Enrollment. However, the birth or adoption of a child is a QLE for a SEP.
Medi-Cal For Pregnant Women Programs
The one exception to all of this are the two programs offered Medi-Cal for women who become pregnant. Medi-Cal For Pregnant covers women’s whose household income is up to 213% of the federal poverty level and the Medi-Cal Access Program for Pregnant women spans the income range of between 213% and 322% of the federal poverty level. (https://www.dhcs.ca.gov/services/medi-cal/Pages/Affordability-and-Benefit-Program.aspx)
Until Covered California fixed the glitch, all women who reported they were pregnant were channeled into the Full Scope Medi-Cal for Pregnant Women program and had their Covered California health plans automatically terminated. This was a nightmare for many families as it completely disrupted their plans for the OBGYN they wanted to see and where they wanted to have their baby delivered.
One of my clients became pregnant and wanted assistance with the costs of the pregnancy through one of the Medi-Cal programs. Under the new Covered California CalHEERS online account system, there are several steps you must take to indicate you want to be considered for Medi-Cal if you indicate you are pregnant.
Switching To Medi-Cal In Covered California
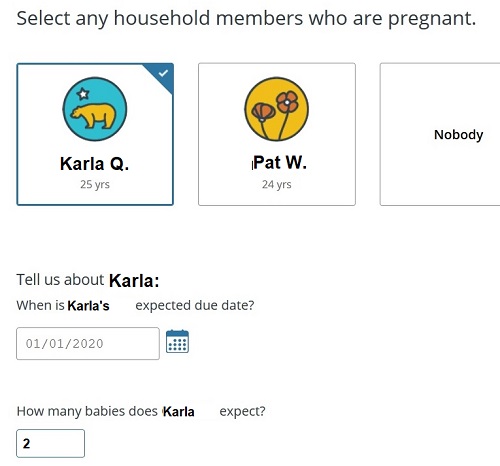
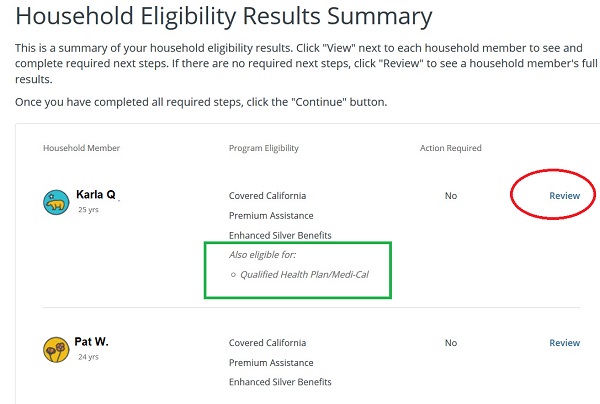
First, the good news, just Reporting a Change that my client was pregnant DID NOT automatically enroll her in Medi-Cal. Unfortunately, the eligibility determination summary doesn’t really scream, “If you want Medi-Cal, click here.” To get to the next level to select Medi-Cal, you have to click the Review link.
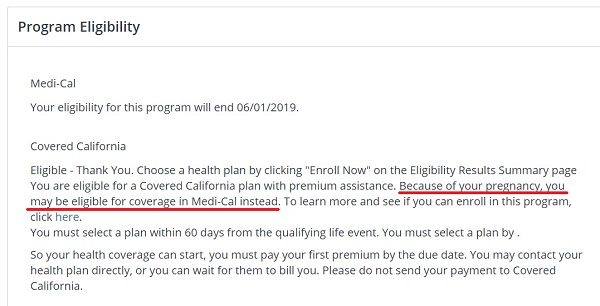
The Program Eligibility page states that because the person has indicated they are pregnant they may be eligible for Medi-Cal. This screen looks as if it was designed for new enrollments and those who are already enrolled and reporting the pregnancy. Hence, some of the verbiage may be slight confusing. The Program Eligibility page also included a date when Medi-Cal eligibility would end. I’m not sure where this date comes from and if that is a hard date at which Medi-Cal must be chosen or forever lost.
Reviewing eligibility report will show individual may be eligible for Medi-Cal 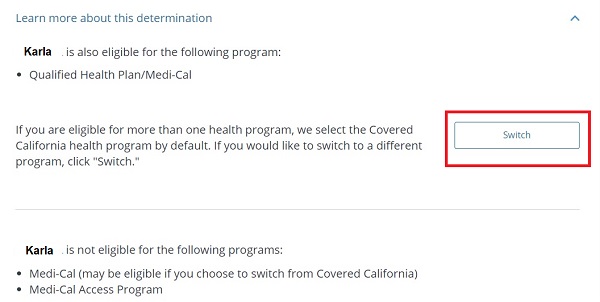
Clicking the Learn more link will provide the button to switch to Medi-Cal.
You have to click on the Learn more about this determination to access the button to make the switch to Medi-Cal. The default enrollment is Covered California, assuming that the household income was above 138% of the federal poverty level to begin with. In my client’s case, both Covered California and I were perplexed why the page indicated the woman was not eligible for Medi-Cal. The household income was clearly in the range for Medi-Cal Pregnant Women.
Even if you indicate you are pregnant, Covered California does not consider the unborn baby a household member for the purposes of determining subsidy eligibility. In this case, even though Karla is pregnant, the subsidy and eligibility is based on a household size of two: Karla and Pat. Medi-Cal does consider a pregnancy an increase in household size. But even with a household of 3, Karla and Pat’s household income was still above 138% of the federal poverty level.
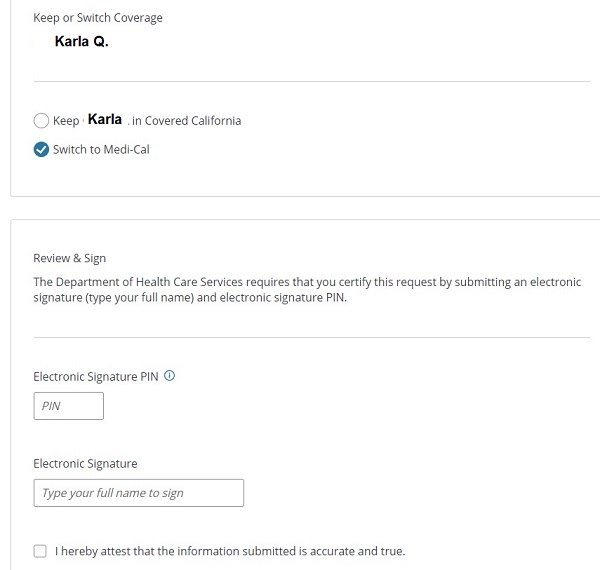
When you click the Switch button, the page expands and you must actively select if you want Medi-Cal and then submit the change as you would do when reporting any other update to the account.
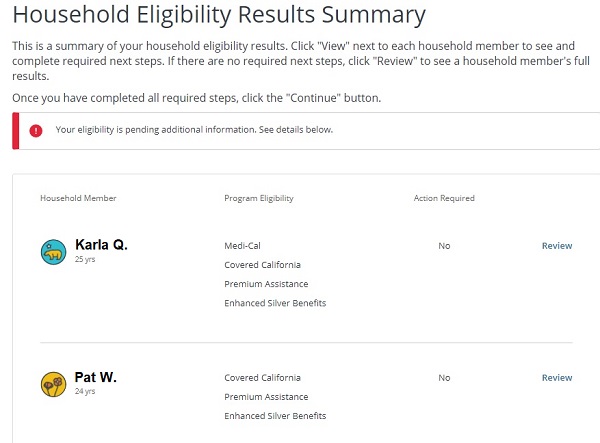
The new Household Eligibility Results showed that Karla was not eligible for Medi-Cal and her spouse was still in the Covered California health plan. Even though the page indicated eligibility was pending additional information, the system was not requesting any other verification documents at that time. I was told that the Covered California system was now sending over the information to the county Medi-Cal office for review and verification, just like any other Medi-Cal eligibility determination.
There still seems to be confusion surrounding the process and the Covered California enrollment, which is understandable. Usually when someone is determined eligible for Medi-Cal, the Covered California system automatically terminates the health plan enrollment. One of the service representatives I talked to at Covered California thought the same would happen in this case, but it did not. The fear was that there might be a lapse in coverage IF the Covered California enrollment was terminated AND Medi-Cal denied enrollment into the one of their pregnancy related programs.
However, when I checked the enrollment status, Karla still was enrolled in her Covered California health plan. While Medi-Cal and Covered California have worked to improve the process over the years, they are still separate enrollment systems with slightly different rules. The updates to the Covered California system help avoid unwanted automatic Medi-Cal enrollment. If the updates work as intended, then just reporting a pregnancy will not trigger a review by the county Medi-Cal office.
But I cannot guarantee that if you report you are pregnant you won’t be contacted by Medi-Cal. They do have a mission to reach out to any potential eligible beneficiary about the many programs they offer.


