
New federal poverty line could put families into Medicaid, Medi-Cal.
The federal Department of Health and Human Services has published the 2015 federal poverty line (FPL) which includes a modest increase over the 2014 FPL. The FPL is used by Marketplace exchanges like Covered California to determine when an individual or family is eligible for either Medicaid, Medi-Cal in California, or tax credits to purchase a private health plan. Household’s whose income qualified them private health plan with tax credits under the 2014 FPL may get knocked into Medi-Cal under the new 2015 FPL.
Federal poverty line increases for 2015
The federal poverty line (FPL) was increased by $100 for an individual in the lower 48 states and Washington D.C from an annual income of $11,670 to $11, 770. In California, household incomes below 138% of the FPL are automatically enrolled into Medi-Cal. For an individual they would need to report and verify an annual income of $16,106 or $1,342.17 per month to be eligible for the Obamacare tax credits. An individual applying for health insurance through Covered California when they implement the new FPL will have to earn approximately $16,244 annually or $1,354 per month to qualify for tax credits.
| Household | 2014 | 2015 | |||
| Size | FPL | >138% | FPL | >138%* | Difference |
| 1 | $11,670 | $16,106 | $11,770 | $16,243 | $137 |
| 2 | $15,730 | $21,709 | $15,930 | $21,984 | $275 |
| 3 | $19,790 | $27,312 | $20,090 | $27,725 | $413 |
| 4 | $23,850 | $32,914 | $24,250 | $33,465 | $551 |
| 5 | $27,910 | $38,517 | $28,410 | $39,206 | $689 |
| 6 | $31,970 | $44,120 | $32,570 | $44,947 | $827 |
| 7 | $36,030 | $49,723 | $36,730 | $50,688 | $965 |
| 8 | $40,090 | $55,326 | $40,890 | $56,429 | $1,103 |
*The 2015 number have been confirmed by a Department of Health Care Services letter to the county welfare directors. Download the letter below-
- [wpfilebase tag=fileurl id=630 linktext=’2015 Medi-Cal Federal Income Poverty Levels’ /]
New FPL could drop families into Medi-Cal
There are many individuals and families that straddle the border line between Medi-Cal and qualifying for the tax credits. Invariably, the 1% increase in the FPL will put some households into the Medi-Cal range. In my conversations with Covered California, individuals and families who were deemed eligible for the tax credits under the 2014 FPL should retain those tax credits if nothing changes with the account. No one could speculate how the individual county social services departments that review Covered California accounts might apply the new FPL income amount to existing income levels. View the 2014 Covered California MAGI household income table at end of post.
Reporting a Change could trigger Medi-Cal eligibility
What is known is that certain changes to a Covered California account automatically trigger a redetermination of eligibility. Not only does reporting a change of income cause the application to be resubmitted for eligibility, but so does a change of address and adding or removing a family member. It is completely possible that a family reporting a new address, even if it is in the same health insurance rating region, could be dropped into Medi-Cal if their income is not adjusted to exceed the new 2015 138% FPL income levels.
Children may be knocked into Medi-Cal
Families with children are also vulnerable to having the children slip into Medi-Cal. Household’s with a Modified Adjusted Gross Income (MAGI) of 266% or less of the FPL will have any children, less than 19 years of age, automatically enrolled in Medi-Cal. If a family of four, two adults and two children, is getting tax credit for all family member’s with a MAGI of $63,450, then reports a change to their household and the new 2015 FPL have been implemented, that original income estimate now puts the children in Medi-Cal. The family would need to adjust their MAGI to $64,506 in order for everyone in the family to qualify for a private health insurance plan.
The new FPL will increase the 266% Modified Adjusted Gross Income level for Medi-Cal Kids.
| Household | Income | <266% |
| Size | Medi-Cal Kids | FPL |
| 2014 | 2015* | |
| 2 | $41,842 | $42,374 |
| 3 | $52,641 | $53,440 |
| 4 | $63,441 | $64,505 |
| 5 | $74,241 | $75,571 |
| 6 | $85,040 | $86,637 |
| 7 | $95,840 | $97,702 |
| 8 | $106,639 | $108,768 |
Medi-Cal SAWS Lock
Some individuals and families who are dropped into Medi-Cal may get locked out of reporting a change to their Covered California account because a lock or hold from Medi-Cal’s Statewide Automated Welfare System (SAWS). “The SAWS is made up of multiple systems which support such functions as eligibility and benefit determination, enrollment, and case maintenance at the county level for some of the state’s major health and human services programs.” – Consolidating California’s Statewide Automated Welfare Systems.
Lock prevents Covered California changes
Covered California has reported that if members of a household are deemed eligible for Medi-Cal they may only have ten days to make changes to get out of the Medicaid program before SAWS places a hold or lock on the account. This lock prevents any changes to the Covered California account that might enable household members to become eligible for tax credits. When this occurs the individual or family must interact with their local county social services department that administers Medi-Cal.
Unlocking SAWS
Melanie Riseley, who has extensive experience with the interface between Covered California and Medi-Cal SAWS, provided the following tips for wrestling with the county to unlock the account.
- The consumer with the frozen account should immediately contact their county representative for Medi-Cal.
- Ask to speak to a supervisor or speak to a qualified staff member who is familiar with how SAWS works.
- Get the contact information from SAWS case worker.
- Request that the household member have their Social Security number released from the SAWS program.
- Attempt to get in writing that the household members has been released.
- Contact Covered California to confirm they’ve been released.
- Advise the Covered California Service Center Representative that you would like to have reinstatement of the carrier health plan if applicable.
Remember when you and your client are applying for medical insurance, you’re doing so under penalty of perjury – your signature confirms the truthfulness of your answers; you should notify the exchange should you discover mistakes on your application or if you’ve reported changes to the county.
Systems don’t talk to each other
For all the technological wizardry of the Covered California CalHEERS enrollment system and the Medi-Cal SAWS program, request for changes can still take weeks. In the most diplomatic language I can muster, there are both county Medi-Cal case workers and Covered California customer service representatives who really don’t understand how their systems work. In other words, some of these folks just don’t know how to process the paper work to move a family out of Medi-Cal and back to Covered California even when presented with all the information and documentation. It’s important that you find the most competent and experienced person to handle unlocking the Medi-Cal case.
Prepare for long wait times
As Covered California updates their federal poverty line income amounts, consumers and agents need to pay particular attention to the details when they make changes to the household account. Always compare the current estimated MAGI to the Covered California income table to make sure that reporting a change won’t inadvertently drop some or all of the household members in Medi-Cal; if in fact they are eligible for the Advance Premium Tax Credits to purchase a private health plan.
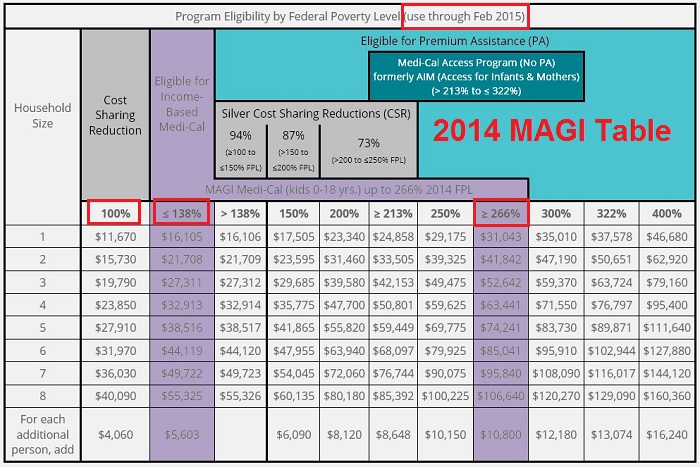
Covered California 2014 Modified Adjusted Gross Income table for Medi-Cal eligibility.


