When the Covered California system is in the renewal mode, changes to your household will affect enrollment and subsidies for 2020. If you need to make changes for 2019, you will want to go through the Report A Change function on the home page.

Kevin Knauss: Health, History, Travel, Insurance
Posts pertaining to issues regarding enrollment in Covered California, Medi-Cal, Medicare, resolving problems.



It is not intuitive that a person who is not automatically enrolled in Medicare must contact the Social Security Administration (SSA). However, the SSA is the gatekeeper of your employment and income records and therefore can make the determination of who is eligible for Medicare based on their work history.


The Special Enrollment Period, Qualifying Life Events, and changes to income are VERY date sensitive. It can also be a little confusing in terms of what dates to use. If you don’t enter the correct dates, such as when income stopped or started, the application process can go sideways and you might be determined eligible for Medi-Cal. When in doubt, call your agent or the Covered California customer service line to determine the correct dates for your qualifying life event.


The Medi-Cal representatives also confirm that erroneous information can pop into Covered California applications after an individual or family has been terminated from Medi-Cal. Once a person is deemed no longer eligible for Medi-Cal, the SAWS Soft Pause is released and the individual and family can then enroll in a Covered California plan with the tax credit subsidy. Unfortunately, the data on the Covered California can be missing or in accurate from what was originally entered.


You must have been enrolled in a Medicare Advantage medical plan to take advantage of the MA OEP. If you never enrolled in a MA or MA-PD, you can’t join one during the MA OEP. You can’t switch standalone Part D Prescription drug plans during the MA OEP. Additionally, if you go from a MA-PD to a MA plan, you can’t add a standalone Part D Prescription Drug plan. The MA OEP doesn’t apply to Medicare Savings Accounts (MSAs) or Cost Plans.


When I looked at the submitted application – there it was – I had to have selected the permanently moved to California QLE which is below loss of coverage. The permanent move to California QLE triggers the standard effective date of the 1st of the following month, in this case August 1st. So the family really did not have insurance for July!

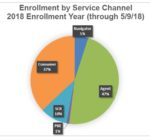
The increased revenue is also in light of reducing health plan assessment from 4% of the gross premiums down to 3.75% for the individual and family plan market. The proposed operating budget for FY 2018-19 is $340.2 million. This represents a 6.55 increase over the FY 2017-18 budget or an increase of $20,686,242.


Because Peter did not have health insurance in the last 60 days, he technically doesn’t qualify to enroll in a health plan in California. But when Peter moves out to California, his job has not started and he has no monthly income, he is just living off of his savings until the job starts in early summer. Because Peter has no monthly income, he qualifies for MAGI Medi-Cal.



Both Health Net and Blue Shield have wasted thousands of hours of time for consumers, agents, and their customer service staff. Tempers have become short and patience has run thin. And as of December 21st, a month after some people have applied for health insurance, 10 days before the plans are to become effective, many families don’t know if they will have insurance on January 1, 2018.

Spam prevention powered by Akismet